Table of Contents >> Show >> Hide
- What “Herpes” Usually Means (and What It Doesn’t)
- Symptoms: What Herpes Can Look and Feel Like
- Causes and How Herpes Spreads
- Diagnosis and Testing: How to Know What You’re Dealing With
- Treatment: What Actually Helps (and What Helps You Cope)
- Prevention and Reducing Transmission Risk
- Herpes and Pregnancy: Special Situations, Higher Stakes
- Common Myths (Let’s Retire These for Everyone’s Sanity)
- Living With Herpes: The Part People Don’t Teach in Health Class
- Real-Life Experiences: What It Can Feel Like (and How People Work Through It)
- Conclusion
“Herpes” is one of those words that can make people panic-scroll at 2 a.m. (right between “why is my toe twitching?” and “is it normal to Google symptoms in the dark?”). Take a breath: herpes simplex is common, often manageable, andwhile it can be emotionally loudmedically it’s usually a condition you learn to handle with the right information, support, and treatment plan.
This guide breaks down herpes symptoms (síntomas), causes (causas), and treatment (tratamiento) in clear American English, with practical examples and a stigma-free approach. It’s educationalnot a substitute for careso if you have symptoms, concerns about a partner, eye pain, pregnancy, or a newborn involved, a clinician is the best next step.
What “Herpes” Usually Means (and What It Doesn’t)
In everyday conversation, “herpes” typically refers to herpes simplex virus infectioneither HSV-1 or HSV-2. HSV-1 is often associated with oral herpes (cold sores), and HSV-2 is more often associated with genital herpes. But here’s the plot twist: either type can affect the mouth or the genitals. That’s why providers may talk about “HSV-1 genital infection” or “HSV-2 oral infection” instead of relying on old labels.
Also: herpes simplex is not the same thing as shingles (herpes zoster). They’re in the same broader virus family, but shingles comes from varicella-zoster virus (the chickenpox virus). Different virus, different situation, different treatment conversations.
The big concept to understand is latency. After the first infection, HSV settles into nearby nerve cells and can go “quiet” for long stretches. Later, it can reactivate (think: the world’s least-welcome pop-up notification), causing symptoms againor causing no symptoms while still shedding virus.
Symptoms: What Herpes Can Look and Feel Like
The “heads-up” phase (prodrome)
Many people notice a warning period before sores appear. Common prodrome symptoms include tingling, itching, burning, or tenderness in the area where sores may develop. This can last hours to a day or two. For some, this is the moment to start “episodic” antiviral medication (if prescribed), because timing can matter.
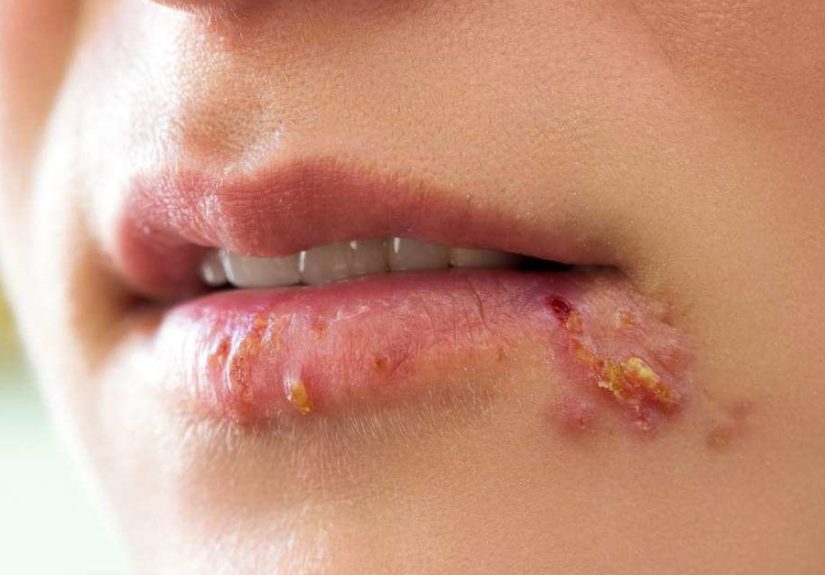
Oral herpes (cold sores)
Oral herpes often shows up as clusters of small blisters near the lips or around the mouth. They can break open, ooze, crust, and heal over about 1–2 weeks. Some people only get a single sore; others get a cluster. You might also feel swelling, tenderness, or mild pain. A first outbreak can be more intense and may come with fever or sore throat.
Example: You feel a “sunburn-y tingle” on the edge of your lip Monday afternoon. By Tuesday morning, a few tiny blisters show up like they’re auditioning for a drama series. That’s a classic pattern many people report.
Genital herpes
Genital herpes symptoms can include pain or itching around the genitals, anus, buttocks, or upper thighs; small bumps or blisters; and painful ulcers if blisters break. Some people have painful urination (especially if sores are near the urethra) or swollen groin lymph nodes. The first episode can be accompanied by flu-like symptoms such as fever, body aches, or fatigue.
Many people also have mild symptoms or none at all. Mild outbreaks can be mistaken for razor burn, ingrown hairs, a pimple, or a friction irritation. That confusion is a big reason herpes often goes undiagnosed.
First outbreak vs. recurrences
The first recognized outbreak tends to be the most intense and longest. Recurrent outbreaks are often shorter and milder over time, though frequency varies a lot. Some people have several outbreaks a year; others have rare or no noticeable recurrences.
When symptoms need urgent attention
Call a clinician promptly (or seek urgent care) if you have:
- Eye symptoms (pain, light sensitivity, blurred vision, redness)HSV can affect the eye and needs fast evaluation.
- Severe headache, confusion, stiff neckrarely, HSV can cause serious nervous system infection.
- A newborn with fever, lethargy, poor feeding, rash, or unusual behaviornewborn infections are emergencies.
- Weakened immunity (e.g., certain medications or conditions) and new/worsening sores.
Causes and How Herpes Spreads
HSV spreads through direct skin-to-skin contact with an infected area, usually via mucous membranes or tiny breaks in the skin. For oral herpes, that might be kissing or sharing saliva during close contact. For genital herpes, it’s often vaginal, anal, or oral sex.
Here’s a key fact that clears up a lot of confusion: herpes can spread even when there are no visible sores. This is called asymptomatic shedding. It doesn’t mean you’re contagious all the time, but it does mean “no symptoms” doesn’t always equal “no risk.”
Factors that can increase the chance of outbreaks (reactivation) include illness, stress, sleep disruption, friction/irritation, sun exposure (especially for cold sores), and hormonal changes. Not everyone has identifiable triggerssometimes HSV reactivates just because it can.
Diagnosis and Testing: How to Know What You’re Dealing With
If you have an active sore, the most straightforward way to confirm herpes is to have a clinician swab the lesion. Many clinics use PCR testing because it detects viral genetic material and is generally faster and more accurate than older methods like viral culture. Viral culture may still be used, but it can be less sensitiveespecially if the sore is already healing.
If you don’t have sores at the moment, blood tests can look for type-specific antibodies (usually HSV-1 or HSV-2 IgG). But blood tests can be tricky: results may be negative early after exposure, and false positives can happenespecially in lower-risk people. That’s why many public health recommendations do not encourage routine blood-test screening for herpes in people without symptoms.
A practical rule: test when it will change your care. Testing is often most useful when you have symptoms, a partner with known herpes, you’re pregnant with relevant history, or a clinician sees something suspicious that needs confirmation.
What to ask your clinician
- Is this consistent with herpes, or could it be something else (yeast infection, bacterial infection, dermatitis, syphilis, etc.)?
- If swabbing, are you using PCR?
- If blood testing, is it type-specific (HSV-1 vs HSV-2), and how should we interpret a low-positive result?
- What’s the best plan for episodic vs suppressive treatment in my situation?
Treatment: What Actually Helps (and What Helps You Cope)
There’s no cure that removes HSV from the body, but there are highly effective antiviral medications that can: reduce symptom severity, speed healing, lower outbreak frequency, and reduce (not eliminate) transmission risk.
Prescription antivirals
The standard oral antivirals include acyclovir, valacyclovir, and famciclovir. Providers generally use them in two main ways:
- Episodic therapy: You take medication at the first sign of an outbreak (or during prodrome). This works best when started early.
- Suppressive therapy: You take medication daily to reduce the number of outbreaks and lower transmission risk, especially with frequent recurrences or significant distress.
Which approach fits best depends on outbreak frequency, relationship context, pregnancy considerations, and personal preference. Some people use suppressive therapy during certain seasons (stressful work periods, new relationship) and episodic therapy at other timesunder clinician guidance.
Over-the-counter options and comfort care
For cold sores, an OTC antiviral cream containing docosanol can help some people when used early. For comfort, many people also use: cool compresses, gentle cleansing, and pain relievers (as appropriate). For genital outbreaks, practical comfort steps may include loose clothing, keeping the area dry, and warm sitz baths. The goal is to reduce irritation while your immune system and treatment do the heavy lifting.
What not to do
- Don’t pick at sores. It can worsen irritation and prolong healing.
- Don’t apply random harsh products (strong acids, essential oils, etc.) to lesions. If it burns like betrayal, it’s probably not helping.
- Don’t assume it’s “just a pimple” if it’s recurring or painfulget it checked.
Prevention and Reducing Transmission Risk
Herpes risk reduction is about layering protectionsbecause no single step is perfect on its own.
During outbreaks: take the obvious win
Avoid kissing (for oral herpes) or sexual contact (for genital herpes) when sores are present or when you feel prodrome symptoms. This is the highest-risk time.
Barrier methods help, but aren’t magic shields
Condoms and dental dams can lower transmission risk, but they don’t eliminate it, because herpes can shed from skin that isn’t covered. Still, consistent barrier use is a meaningful toolespecially combined with good communication and medical treatment when appropriate.
Suppressive therapy and partner protection
Daily suppressive antivirals can reduce outbreak frequency and lower the risk of passing HSV to a partner. This option is commonly discussed for people with recurrent HSV-2, and sometimes for HSV-1 genital infection if recurrences are frequent.
Talk about it (yes, really)
A conversation can feel scarier than a swab test, but it’s often the most empowering part of managing herpes. Many couples do best when they treat it like any other shared health decision: discuss timing, protection preferences, testing, and comfort level.
A simple script that doesn’t sound like a legal disclaimer:
“I want to share something health-related before we get closer physically. I have herpes (HSV-__). Most of the time I have no symptoms, but it can still spread sometimes. There are ways to reduce risklike condoms and (if needed) daily medication. I’m happy to talk through what feels comfortable for both of us.”
Herpes and Pregnancy: Special Situations, Higher Stakes
Pregnancy changes the risk calculation because herpes can be passed to a baby during delivery, especially if a person acquires genital herpes late in pregnancy or has active lesions at delivery. That doesn’t mean panicit means planning.
If you’re pregnant (or planning to be), tell your obstetric provider if you have a history of genital herpes or suspect exposure. Providers may recommend antiviral suppression in late pregnancy for those with recurrent genital herpes, and they carefully assess symptoms near delivery. If active genital lesions or prodromal symptoms are present at labor, cesarean delivery may be recommended to reduce neonatal risk.
Common Myths (Let’s Retire These for Everyone’s Sanity)
Myth: “Only people with lots of partners get herpes.”
Reality: herpes is common. One partner can be enough. Sometimes transmission happens from someone who has no idea they carry HSV.
Myth: “If there are no sores, there’s no risk.”
Reality: asymptomatic shedding is real. Symptoms raise risk, but absence of symptoms doesn’t guarantee absence of virus.
Myth: “A standard STI panel always includes herpes.”
Reality: many routine panels don’t automatically include herpes blood tests. If herpes testing matters in your situation, ask specifically.
Myth: “Condoms eliminate herpes risk.”
Reality: condoms reduce risk, but don’t fully eliminate it because of uncovered skin shedding. They’re still a strong part of risk reduction.
Myth: “Herpes ruins your dating life.”
Reality: plenty of people have healthy relationships and sex lives with HSV. The emotional weight is often heavier than the medical realityand both are treatable: one with antivirals and care, the other with knowledge, support, and (sometimes) therapy.
Living With Herpes: The Part People Don’t Teach in Health Class
If you’re newly diagnosed, the first week can feel like your brain is hosting a 24/7 talk show titled “What Does This Mean About Me?” But herpes is a virus, not a personality trait.
What helps most people long-term looks surprisingly practical:
- Get clear on your type (HSV-1 vs HSV-2) and location (oral vs genital). It helps with expectations about recurrences.
- Have a plan: an episodic prescription on hand (if appropriate), or suppressive therapy if outbreaks are frequent or distressing.
- Learn your triggers (if you have them): stress, sleep disruption, friction, sun exposure.
- Build your disclosure style: simple, honest, and centered on shared decisionsnot shame.
- Protect your mental health: stigma is loud; facts are louder when you keep them close.
And yes, humor can be part of coping. Many people find it helpful to reframe HSV as “a manageable skin/nerve virus that occasionally sends a calendar invite you didn’t accept.” The point isn’t to dismiss feelingsit’s to make space for the reality that you can live normally.
Real-Life Experiences: What It Can Feel Like (and How People Work Through It)
People’s experiences with herpes vary widely, but certain themes come up again and againespecially around first symptoms, diagnosis, and learning how to talk about it. Many describe the first outbreak as the moment everything feels amplified: physical discomfort plus emotional noise. Someone might notice a tingling sensation, then see a small cluster of blisters and immediately assume the worst. The waitingwaiting for an appointment, waiting for test resultsoften feels harder than the sores themselves.
After diagnosis, a common experience is a sharp spike of shame that doesn’t match the medical facts. People say things like, “I felt dirty,” or “I thought no one would want me.” In reality, clinicians see HSV constantly, and millions of adults live with it. The emotional reaction isn’t “overdramatic”it’s human. What helps is replacing vague fear with specific knowledge: which virus type it is, how it spreads, what outbreaks look like for you, and what treatment options exist.
Many people also describe a shift from “reacting” to “managing.” At first, outbreaks can feel random and unfair. Over time, some start noticing patterns: cold sores after a beach weekend without SPF lip balm, genital symptoms after a week of little sleep and big stress, or flare-ups when friction and irritation are higher. Others never identify a clear triggerand that’s normal too. The key experience is learning that outbreaks don’t mean failure; they’re simply part of how HSV behaves in the body.
Dating and relationships are another major chapter. A lot of people fear disclosure like it’s a high-stakes courtroom drama, but many report that calm, honest conversations go better than expected. Some partners already know about HSV from past experience. Some ask thoughtful questions. Some need time to processand that’s okay. The experience that tends to feel best long-term is choosing partners who can handle adult conversations about health.
For those in long-term relationships, herpes often becomes “background noise.” Couples may decide on condoms, daily suppressive medication, or simply avoiding sex during outbreaks. They learn what prodrome feels like, keep medication accessible if prescribed, and move on with life. The virus remains, but it stops being the headline. People who become pregnant often describe a fresh wave of worrythen relief after talking through a clear plan with their obstetric provider and understanding how risk is managed near delivery.
Finally, many people describe a quiet but real confidence that grows over time: the moment they realize herpes didn’t take their future away. They still have careers, families, relationships, and a body that deserves kindness. If there’s one “shared experience” thread, it’s this: once you have accurate information and a plan, herpes becomes a manageable part of your healthnot a definition of who you are.
Conclusion
Herpes (HSV) is common, often subtle, and highly manageable. Understanding the symptoms, how transmission works (including asymptomatic shedding), and how testing and treatment fit together can turn a scary mystery into a practical plan. If you think you might have herpesor you simply want claritytalk with a clinician. Getting accurate information is the fastest route back to peace of mind.






