Table of Contents >> Show >> Hide
- Does Medicare cover EYLEA? Usually yesunder the right “bucket”
- What EYLEA is (and why retina specialists love it)
- How Original Medicare pays for EYLEA injections
- Medicare Advantage: the same medication, more hoops
- What can make EYLEA coverage get denied (or delayed)?
- Ways to lower what you pay
- EYLEA HD and biosimilars: what changes (and what doesn’t)
- How to verify coverage before your next injection
- Conclusion
- Experiences: what Medicare + EYLEA “feels like” in real life (and how to make it easier)
If you (or someone you love) gets EYLEA (often misspelled “Eyelea”) injections for a retinal condition,
you’ve probably learned two things: (1) modern eye medicine is amazing, and (2) insurance paperwork can make you need a second prescription
for aspirin.
The good news: Medicare often covers EYLEA when it’s medically necessary. The “complicated” news: what you pay depends on
which type of Medicare you have (Original Medicare vs. Medicare Advantage), where you receive treatment (doctor’s office vs. hospital outpatient),
whether you carry supplemental coverage, and whether the claim is coded and documented correctly.
This guide breaks it all down in plain Englishwith real-world examples, common billing codes you may see,
and a few practical tips to keep your eyesight cared for and your budget less… jumpy.
Does Medicare cover EYLEA? Usually yesunder the right “bucket”
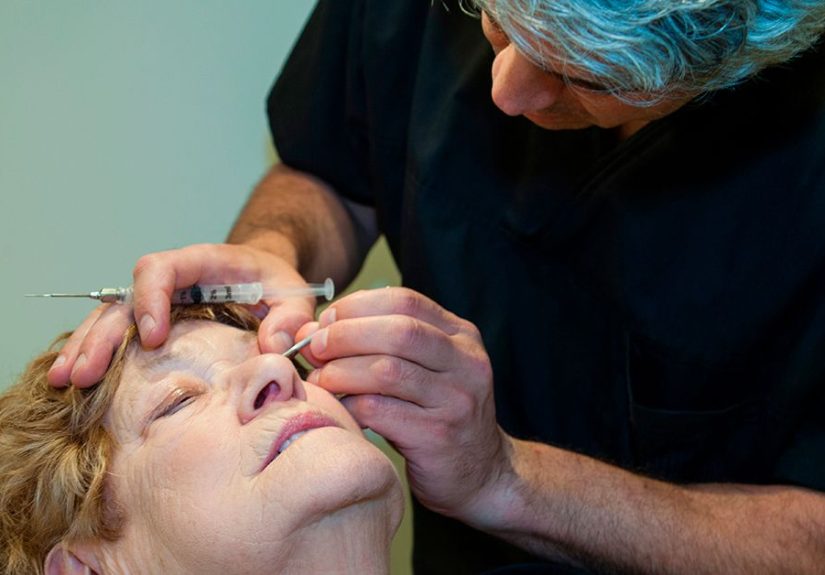
EYLEA (aflibercept) is an intravitreal injectiona medication injected into the eyemost often used to treat conditions like:
wet age-related macular degeneration (wet AMD), macular edema after retinal vein occlusion (RVO), diabetic macular edema (DME),
and diabetic retinopathy (DR).
Because EYLEA is typically administered by your retina specialist in a clinic (not taken at home like a pill),
it’s generally covered as a Medicare Part B drugnot Part D.
The simplest rule of thumb
- Original Medicare (Part A + Part B): EYLEA is usually covered under Part B when medically necessary.
- Medicare Advantage (Part C): The plan must cover Part A and Part B services, but it may require prior authorization, use step therapy, or have network rules.
- Part D: Usually not the main payer for EYLEA injections, since the drug is administered in-office.
What EYLEA is (and why retina specialists love it)
EYLEA is a VEGF inhibitor (anti-VEGF therapy). In several retinal diseases, your eye produces too much VEGF,
which contributes to leaky blood vessels, swelling, bleeding, and vision loss. Anti-VEGF injections help reduce leakage and swelling,
which can stabilizeand sometimes improvevision.
Medicare coverage hinges on a concept called medical necessity. If your diagnosis and treatment match accepted indications and
clinical standards, coverage is typically straightforward. If documentation is thin, coding is off, or the plan wants prior authorization,
that’s when things get… spicy.
How Original Medicare pays for EYLEA injections
Part B vs. Part D: why this matters for your wallet
Medicare Part B generally covers drugs that are not usually self-administered and are furnished as part of, or “incident to,”
a physician’s service. Intravitreal injections fit that pattern.
Translation: EYLEA is usually billed like other outpatient physician-administered drugs. That means your costs often look like other Part B services:
deductible first, then coinsurance.
What shows up on the claim: common codes (the “translation key”)
When your retina clinic bills Medicare, you may see a few different line items. The exact mix varies by setting, but these are common:
-
The drug code (what medication was used). For EYLEA (aflibercept), billing often uses a HCPCS “J-code” or “Q-code.”
You might see different codes depending on dose formulation (standard vs. high-dose) and whether a biosimilar is used. -
The injection procedure (the act of injecting the medication). A common CPT code for intravitreal injection is
67028. -
Which eye (right, left, or both). Modifiers like RT and LT may be used,
and bilateral billing has payer-specific rules. - Office visit (if separately billable) and imaging (like OCT) when medically necessary.
Why should you care? Because a surprising number of “coverage problems” are actually billing or documentation problemsfixable,
but only if you know what you’re looking at.
Coverage criteria: “reasonable and necessary” plus documentation
Medicare coverage isn’t just “drug = covered.” Contractors often rely on national guidance and local coverage policies to determine whether the drug is
reasonable and necessary for your condition, and whether dosing frequency makes sense for that diagnosis.
In practice, your retina specialist typically documents things like:
- Diagnosis (for example, wet AMD, DME, or macular edema after RVO)
- Clinical findings (symptoms, exam findings, visual acuity)
- Imaging such as OCT when relevant
- Treatment plan (initial series, follow-up interval, response)
- Why EYLEA (especially if a plan wants step therapy or you’re switching agents)
If any of these pieces are missing, a claim can be delayed, denied, or kicked back for additional informationespecially under Medicare Advantage.
What you typically pay with Original Medicare
Under Original Medicare Part B, you generally pay:
- Part B deductible (once per year, if you haven’t already met it)
- 20% coinsurance of the Medicare-approved amount for covered Part B services
Here’s the part that catches people off guard: EYLEA is a specialty drug and can be expensive. So even 20% can feel like a punchy little surprise.
A simple example (numbers made up, but the math is real)
Let’s say the Medicare-approved amount for an injection visit (drug + injection procedure + related services) is $2,000.
After you’ve met your deductible, your share under Original Medicare could be about $400 (20%).
That’s why supplemental coverage can make such a big difference.
Important note: Medicare-approved amounts can vary by setting (office vs. hospital outpatient), region, and drug pricing updates.
Your clinic’s billing team can often estimate your out-of-pocket cost before treatment if you ask.
Medicare Advantage: the same medication, more hoops
Medicare Advantage plans (Part C) must cover at least what Original Medicare covers, but they can manage access through tools like:
prior authorization, step therapy, and network requirements.
Prior authorization: why it happens
EYLEA injections are high-value care, but they’re also high-cost care, so they’re exactly the sort of service plans tend to scrutinize.
Many Medicare Advantage enrollees are in plans that require prior authorization for certain servicesoften including Part B drugs.
The practical reality: your retina clinic may need to send records showing your diagnosis, imaging, prior treatments, and planned dosing schedule.
If the paperwork is complete, approvals can be routine. If it’s incomplete, you may see delays.
Step therapy: “try this first” policies
Some plans prefer certain anti-VEGF agents (or biosimilars) before others. That doesn’t automatically mean you can’t get EYLEA,
but it may mean your doctor has to explain why EYLEA is appropriateespecially if:
- You didn’t respond well to another agent
- You had side effects
- You need a specific dosing interval
- You’re switching due to clinical response, not convenience
Network and site-of-care can change your cost
With Medicare Advantage, using an in-network retina specialist and approved facility can matter a lot.
A visit in a hospital outpatient department may involve different cost-sharing than an in-office injectionso ask where the claim will be billed.
What can make EYLEA coverage get denied (or delayed)?
Most patients don’t get denied because EYLEA is “never covered.” The usual culprits are more boringand more fixable:
1) Coding and unit errors
- The wrong drug code (standard vs. high-dose vs. biosimilar)
- Incorrect units billed (the drug is billed by unit dose)
- Missing RT/LT modifiers or payer-required billing format
2) Documentation gaps
- Diagnosis not clearly linked to the treatment
- Missing imaging notes or test interpretation (when relevant)
- No rationale for dosing frequency or switching agents
3) Plan rules (mostly Medicare Advantage)
- No prior authorization on file (or it expired)
- Step therapy requirement not met (or not documented)
- Out-of-network provider or facility without approval
If your bill looks off, ask for an itemized statement and compare it to your Medicare Summary Notice (Original Medicare)
or your Explanation of Benefits (Medicare Advantage). Many issues can be corrected with a claim resubmission.
Ways to lower what you pay
Medigap (Medicare Supplement): the “quiet hero” for Part B coinsurance
If you’re on Original Medicare, a Medigap policy may help cover your share of Part B costs (like the 20% coinsurance).
The exact coverage depends on the plan letter you choose.
In plain terms: for expensive Part B drugs, Medigap can be the difference between “manageable” and “I suddenly understand minimalism.”
Manufacturer support: helpful, but watch eligibility rules
Drug manufacturers often provide patient support services (benefit verification, education, andsometimesfinancial assistance).
However, copay cards are generally designed for commercially insured patients, not for people on government insurance.
That doesn’t mean you’re out of options; it does mean you should ask the program what assistance is available for Medicare beneficiaries
(often it’s more about navigation support, foundations, or other pathways than direct copay-card help).
Quarterly coinsurance reductions for certain Part B drugs
Medicare has mechanisms that may reduce coinsurance for some Part B drugs when certain price increases exceed inflation thresholds.
The specific drugs and savings can change quarterlyso it’s worth asking your clinic’s billing team if any reductions apply.
EYLEA HD and biosimilars: what changes (and what doesn’t)
EYLEA HD (higher dose)
EYLEA HD is a higher-dose formulation of aflibercept. Clinically, higher-dose options may allow some patients to stretch time between injections
after an initial phasemeaning fewer trips to the retina clinic (which patients generally love).
From a Medicare perspective, the big picture is similar: it’s still typically a physician-administered intravitreal drug covered under Part B
when medically necessary. What can change is the billing code, dose units, and the plan’s preferred product rules.
Biosimilars: same category, different code
Biosimilars to aflibercept are entering the market, and Medicare billing may use different “Q-codes” for these products.
Some Medicare Advantage plans may prefer a biosimilar for cost reasonssimilar to how plans prefer generics when available.
Practically, this is a conversation for your retina specialist:
“Is a biosimilar clinically appropriate for me?” If yes, it may reduce costs. If no, your doctor can document why the reference product
(EYLEA) is medically necessary.
How to verify coverage before your next injection
Here’s a checklist you can useespecially if you have Medicare Advantage or you’ve had a surprise bill before.
Ask your retina clinic’s billing team
- Is the injection billed under Part B?
- What drug code will you use (standard EYLEA vs. EYLEA HD vs. biosimilar)?
- Is prior authorization needed for my plan?
- Will the claim be billed as an office service or hospital outpatient?
- Can you estimate my out-of-pocket cost?
Ask your plan (especially Medicare Advantage)
- Do I need prior authorization for intravitreal anti-VEGF injections?
- Is EYLEA covered for my diagnosis (wet AMD, DME, RVO, DR)?
- Is there a preferred agent or step therapy requirement?
- Do I need to use specific in-network facilities?
Keep your paperwork (yes, really)
Save your Medicare Summary Notices or plan EOBs. If something is denied, your appeal is stronger when you can show consistency of diagnosis,
response to therapy, and medical necessity over time.
Conclusion
Medicare and EYLEA coverage doesn’t have to be a mystery novel with missing pages. In most cases, EYLEA is covered under Part B
when it’s medically necessary and documented correctly. Your biggest “swing factors” are whether you have Original Medicare vs. Medicare Advantage,
whether you carry Medigap or other supplemental coverage, and whether the plan requires prior authorization or step therapy.
If you only remember three things, make them these:
(1) ask your clinic to estimate your cost before treatment,
(2) confirm prior authorization if you’re on Medicare Advantage,
and (3) don’t panic over a denial until you’ve checked for coding and documentation issuesbecause many are fixable.
Experiences: what Medicare + EYLEA “feels like” in real life (and how to make it easier)
The clinical part of EYLEA treatment is usually quick: check-in, vision test, maybe an OCT scan, a conversation with the doctor, then the injection.
The emotional part? That can stretch out over weeksespecially when the billing side joins the chat.
One common experience is “the sticker-shock moment”. A patient on Original Medicare may assume that because Medicare covers the injection,
it’ll be cheap. Then a bill arrives showing a 20% coinsurance on a high-cost drug. Even when everything is billed correctly, the out-of-pocket share
can be surprising. People often describe it as: “The injection didn’t hurt. The statement did.” This is where Medigap (or other secondary coverage)
changes the experience dramaticallysome patients go from dreading the mailbox to barely thinking about it.
Another frequent storylineespecially for Medicare Advantageis the prior authorization relay race. The doctor recommends treatment,
the clinic submits paperwork, the plan asks for one more page, the clinic resubmits, the plan requests a different form, and suddenly you’re
emotionally invested in a fax machine you’ve never met. Clinics that do retina injections all day are used to this and often have dedicated staff.
But delays can still happen, and patients often feel stuck in the middle. The best move is surprisingly simple:
ask the clinic whether authorization is approved before the appointment, and if it isn’t, ask what’s missing.
Sometimes one missing OCT note or diagnosis code is the whole problem.
Then there’s the “left eye vs. right eye” billing confusion. Intravitreal injections are billed per eye, and claims may use RT/LT modifiers
or other payer-specific formats. Patients occasionally see denials that look scary but boil down to “wrong modifier” or “units don’t match.”
It’s annoying, but it’s also fixableusually by the clinic resubmitting the claim with corrected details. This is why requesting an itemized statement
is such a power move: you’re not arguing about medicine; you’re matching line items to what actually happened.
A quieterbut very realexperience is the treatment cadence. Many retinal diseases require ongoing injections, and patients often describe
their calendars as “built around eye day.” When a therapy plan allows longer intervals (when clinically appropriate), patients frequently report that it
improves their quality of lifenot just fewer appointments, but less travel stress, fewer rides to coordinate, and fewer days of post-injection caution.
If your doctor discusses extending intervals, it’s okay to ask, “Is this clinically safe for me?” and also, “Will my plan treat this differently?”
(Most of the time, coverage follows medical necessitybut plans can be picky about documentation.)
Finally, many patients say the biggest relief comes from realizing they’re allowed to be proactive. Calling the plan once, asking the clinic for a cost estimate,
and understanding that EYLEA is usually a Part B benefit turns the process from confusing to manageable. You don’t need to become a billing expert.
You just need a short script: “Is this authorized? What code are you using? What will I owe?” That’s the difference between feeling powerless
and feeling prepared.






