Table of Contents >> Show >> Hide
- The Big Headline Is Real, but It Needs Context
- Why GLP-1 Weight Loss Drugs Are Changing the Story
- The Uptake Has Been Fast Enough to Move National Numbers
- Why the Decline Does Not Mean Obesity Is “Fixed”
- The Drug Boom Is Also Creating New Risks
- What This Means for the Future of the U.S. Obesity Rate
- What Real-World Experiences With Ozempic and Similar Drugs Actually Look Like
- Conclusion
Note: Body-only HTML draft for direct publishing. Source links are intentionally omitted by request.
Note: This is a body-only HTML article in standard American English, ready to paste into a CMS or webpage editor.
For years, America’s obesity story had all the cheerful energy of a smoke alarm at 3 a.m.: loud, relentless, and impossible to ignore. Rates kept climbing, doctors kept warning, and public health experts kept saying the same thing in increasingly urgent fonts. Then, almost quietly, a different headline started to appear. The U.S. obesity rate may finally be inching down. Not collapsing. Not vanishing. Not riding a bald eagle into the sunset. But moving in the right direction.
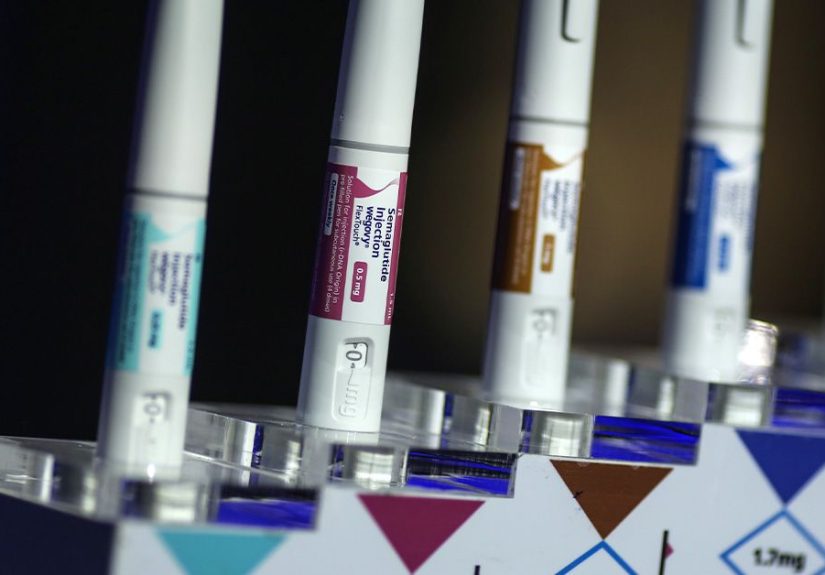
The timing is hard to miss. As GLP-1 weight loss drugs like Wegovy and Zepbound surged into mainstream medicineand as Ozempic became the catch-all celebrity nickname for the whole conversationobesity numbers began to show signs of softening. Gallup reported that the self-reported U.S. adult obesity rate fell from a record 39.9% in 2022 to 37.0% in 2025, a meaningful drop that translates to millions fewer adults classified as obese. A separate analysis in JAMA Health Forum also found that body mass index and obesity prevalence appeared to decline in 2023 for the first time in more than a decade.
That does not mean the crisis is over. It means the map may finally have a corner that is no longer on fire.
The Big Headline Is Real, but It Needs Context
Let’s start with the most important reality check: America is still a very obese nation. The Centers for Disease Control and Prevention reported that obesity affected 40.3% of adults during August 2021 through August 2023. Severe obesity affected 9.4%. Adults ages 40 to 59 had the highest prevalence, and disparities by education remained striking. In 2024, CDC state maps still showed that at least one in four adults in every state and territory had obesity.
So no, this is not a Hollywood makeover montage where the nation drinks a green smoothie, buys matching sneakers, and suddenly fits into old jeans from college. The better way to read the data is this: the long upward climb may be flattening, and in some places it may be beginning to reverse.
That distinction matters because obesity statistics come from different sources and tell slightly different stories. Gallup tracks self-reported obesity. CDC national estimates come from measured health survey data. CDC state maps rely on self-reported height and weight through BRFSS. AP also reported that the number of states with adult obesity rates of 35% or higher fell from 23 in 2023 to 19 in 2024. Encouraging? Yes. Final proof that America has solved obesity? Absolutely not. Even public health leaders have warned it is too soon to call this a lasting trend.
Why GLP-1 Weight Loss Drugs Are Changing the Story
The simplest explanation is that these drugs work better than older obesity medications for many patients. A lot better. GLP-1 receptor agonists mimic gut hormones involved in appetite, fullness, digestion, insulin release, and blood sugar regulation. In plain English, they help people feel less hungry, get full faster, and stop negotiating with the pantry at 10:47 p.m. like it is a hostage situation.
Semaglutide, the active ingredient in Ozempic and Wegovy, has been especially important in this shift. The diabetes version, Ozempic, is FDA-approved for adults with type 2 diabetes and for reducing major cardiovascular events in certain patients with diabetes and heart disease. Wegovy, which also contains semaglutide, is the version FDA-approved for chronic weight management. In 2024, Wegovy also gained an expanded FDA indication to help reduce the risk of serious cardiovascular events in adults with obesity or overweight and established cardiovascular disease.
That approval mattered for two reasons. First, it made the drug more medically compelling to skeptical insurers and clinicians who had previously treated obesity as an aesthetic issue instead of a chronic disease. Second, it helped open the door to Medicare Part D coverage for some patients using Wegovy for cardiovascular risk reduction. In other words, the conversation started shifting from “Should we cover vanity weight loss drugs?” to “Should we ignore a therapy that may prevent heart attacks and strokes?” That is a very different argument.
Ozempic Is the Headline, but Wegovy and Zepbound Are Part of the Real Story
The title says “Ozempic,” because in American culture Ozempic has become a kind of shorthand for the whole GLP-1 era. But the actual public health story is broader. Wegovy is the semaglutide brand specifically approved for obesity, while Zepbound, which contains tirzepatide, is another FDA-approved chronic weight management drug that has rapidly become a major player. Patients and headlines often use “Ozempic” the way people use “Kleenex” for tissues or “Google” for searching. It is not always technically precise, but everyone knows what planet the conversation is on.
Clinical trial results help explain the excitement. Semaglutide studies showed sustained, clinically meaningful weight loss in adults with overweight or obesity. Yale Medicine and other experts now describe these newer anti-obesity medications as a major turning point because they target the biological “set point” mechanisms that make long-term weight loss so hard to maintain through willpower alone. That is one reason the medical community is increasingly framing obesity as a chronic disease, not a personal moral failure with a side of salad guilt.
The Uptake Has Been Fast Enough to Move National Numbers
When enough people start using a highly effective therapy, population-level data can begin to shift. That appears to be what is happening. Gallup found that the share of adults using GLP-1 drugs specifically for weight loss more than doubled, rising from 5.8% in February 2024 to 12.4% in October 2025. KFF separately found that about one in eight adults said they were currently taking a GLP-1 drug in late 2025, whether for weight loss, diabetes, or another condition.
Those are not niche numbers anymore. That is no longer “a few early adopters in Los Angeles and a lot of TikToks.” That is scale. And scale is how a pharmaceutical trend becomes a public health force.
Even research that urges caution hints at the same pattern. The JAMA Health Forum analysis found the most notable decrease in obesity prevalence in the South, where GLP-1 dispensing rates were highest. The authors were careful not to claim a clean one-cause explanation, and they noted other factors could also be involved. Still, the geographic overlap is hard to ignore.
Why the Decline Does Not Mean Obesity Is “Fixed”
This is where the more mature version of the conversation begins. Weight loss drugs may be helping reduce U.S. obesity rates, but they are not a magic wand, a substitute for policy, or a free pass to ignore the social drivers of obesity. A medicine can lower appetite. It cannot build safer neighborhoods, lower food prices, fix sleep deprivation, reduce stress, or make preventive care easier to access.
The CDC’s own data make that plain. Obesity remains far more common among some groups than others, and education-linked differences remain substantial. The burden is not spread evenly. That means the benefits of these drugs may also be uneven unless access improves dramatically.
Access and Affordability Are Still a Mess
This may be the single biggest reason the GLP-1 revolution has not become a full-blown national transformation. KFF reported that list prices for GLP-1 drugs have ranged roughly from $936 to $1,349 before insurance, rebates, or coupons. About half of people who have used GLP-1 drugs have said the medications were difficult to afford. Even among insured adults, many still reported serious cost pressure.
That creates an awkward public health paradox. We now have medications that can meaningfully reduce obesity for many people, improve blood sugar control, and in some cases reduce cardiovascular risk. But the people who may benefit most are often the same people most likely to run into prior authorizations, coverage exclusions, high coinsurance, step therapy rules, or the classic American health care experience known as “your doctor recommends this, but your wallet files an objection.”
Recent Medicare policy changes helped some patients, particularly those eligible for Wegovy because of cardiovascular risk. But broad coverage of anti-obesity medications remains limited and politically contested. Until that changes, the national obesity decline may continue to look less like a universal breakthrough and more like a selective advantage for those who can get through the insurance maze.
Side Effects, Drop-Off, and Weight Regain Are Real
There is also the small matter of biology refusing to be easy. GLP-1 drugs commonly cause nausea, vomiting, diarrhea, stomach pain, constipation, heartburn, or that odd “I am full but also vaguely offended by food” sensation many patients describe early on. Clinicians usually start with low doses and increase gradually to make the process more tolerable, but side effects still push some people to stop treatment.
And stopping can be a problem. In the STEP 1 trial extension, people regained about two-thirds of their prior weight loss within a year after discontinuing semaglutide. That finding reinforced something obesity specialists have been saying for a while: obesity is chronic, and treatment often needs to be chronic too. These are not always “take it for a few months and ride into the sunset” medications. For many patients, they look more like long-term disease management.
That is a big cultural adjustment. Americans are often comfortable taking medicine long term for blood pressure, cholesterol, asthma, and diabetes. But for obesity, there is still a lingering expectation that once a person loses weight, they should somehow “graduate” from treatment and live happily ever after on grilled chicken and discipline. Human metabolism, unfortunately, does not read motivational posters.
The Drug Boom Is Also Creating New Risks
Whenever demand rises faster than access, the sketchier corners of the market start smelling opportunity. FDA has repeatedly warned consumers about unapproved, illegally marketed, or counterfeit GLP-1 products. The agency has said some online products may contain the wrong ingredients, too much or too little active drug, or no active ingredient at all. That is not bargain shopping. That is pharmaceutical roulette.
So while lower-cost access is urgently needed, the “cheap shortcut” ecosystem deserves skepticism. The safest version of this story is still the least glamorous one: a real clinician, a real prescription, a real pharmacy, and realistic expectations.
What This Means for the Future of the U.S. Obesity Rate
The most likely answer is that GLP-1 medications will continue to lower obesity rates gradually, but unevenly. They are effective enough to matter, popular enough to scale, and medically important enough to keep expanding into mainstream care. New formulations, including oral options, may make treatment easier and more acceptable for many patients. Research is also exploring how these drugs perform across age groups, racial and ethnic populations, and different starting body weights, with emerging evidence suggesting they work broadly across many groups, even though individual results still vary a lot.
But the national impact will depend on more than the science. It will depend on who can actually get the drugs, stay on them, tolerate them, and afford them. It will depend on whether insurers keep treating obesity care like optional self-improvement or finally treat it like the chronic disease management it is. It will depend on whether policymakers protect prevention programs at the same time they debate medication coverage. And it will depend on whether the country can resist turning a serious medical shift into yet another celebrity fad narrative.
The smartest takeaway is not that Ozempic “solved” obesity. It is that America may finally have a tool strong enough to push back against it. That is a huge development. It is just not the same as a cure.
What Real-World Experiences With Ozempic and Similar Drugs Actually Look Like
Talk to enough clinicians and patients, and a pattern emerges. The first stage is usually curiosity mixed with skepticism. Someone has struggled with weight for years, sometimes decades. They have counted calories, cut carbs, tried meal plans, joined gyms in bursts of hope, lost some weight, regained it, blamed themselves, and repeated the cycle enough times to deserve frequent flyer miles. Then a doctor mentions semaglutide or tirzepatide. At first, it sounds almost too convenient. An injection? Once a week? And it might quiet hunger? Sure, and maybe the treadmill will also fold my laundry.
Then treatment starts, and many people notice something that feels almost stranger than the weight loss itself: mental quiet. The constant food chatter drops. The background hum of craving gets softer. Meals feel smaller without feeling like punishment. Patients often say they finally understand what doctors meant when they talked about satiety, because for the first time in years, being full actually feels like a real event instead of a clerical error.
But the experience is rarely glamorous. Early weeks can be bumpy. Nausea can make dinner feel unappealing. Constipation can become its own side quest. Some people feel tired. Some discover that eating too fast or too much on these drugs is like trying to negotiate with gravity: you can complain, but you are still going down. The successful patients are often the ones who adjust expectations quickly, eat smaller meals, prioritize protein, hydrate, move their bodies, and stop treating the medication like a solo act. The drug helps, but it does not grocery shop, plan meals, or build muscle on its own.
Then there is the insurance drama, which deserves its own prestige miniseries. Prior authorizations, denials, appeals, shortages, pharmacy scavenger hunts, price shocks, coupon confusion, and the monthly suspense of whether this prescription will cost a manageable amount or the approximate GDP of a small coastal town. For some patients, the treatment works medically but becomes exhausting financially. For others, the biggest anxiety is not the injection but the fear that access will disappear just as life starts to feel more manageable.
Longer term, experiences split. Some patients lose a meaningful amount of weight, improve lab values, feel better in their joints, sleep better, and describe the medication as life-changing. Others plateau and feel frustrated. Some stop because of side effects. Some regain weight after stopping and feel devastated, not because the medicine “failed,” but because it revealed how stubborn biology can be. That may be the most important lived experience of all: these drugs are powerful, but they are not vanity tools for lazy people. They are chronic disease treatments that expose just how physical, persistent, and unfair obesity can be.
And maybe that is the deeper shift behind the numbers. Not just fewer pounds. A different understanding. Less shame, more science. Less “just try harder,” more “let’s treat this seriously.” If GLP-1 drugs continue to bring the U.S. obesity rate down, that may end up being their biggest cultural effect of all.
Conclusion
So yes, the headline holds up: weight loss drugs appear to be contributing to a decline in U.S. obesity rates. But the best version of that headline is the one with a little humility attached. America has not defeated obesity. It has, perhaps, finally found a set of medicines capable of changing the odds. GLP-1 drugs like Ozempic, Wegovy, and Zepbound are shifting the conversation from frustration to possibility, from blame to biology, and from tiny improvements to something that looks like real public health movement. That is not hype. That is a big deal.