Table of Contents >> Show >> Hide
- What Are Splinter Hemorrhages?
- What Do Splinter Hemorrhages Look and Feel Like?
- What Causes Splinter Hemorrhages?
- When Splinter Hemorrhages Are a Warning Sign
- How Doctors Diagnose Splinter Hemorrhages
- Treatments for Splinter Hemorrhages
- How to Protect Your Nails and Lower Your Risk
- Are Splinter Hemorrhages the Same as a Black Line on the Nail?
- When to See a Doctor
- The Bottom Line
- Real-World Experiences With Splinter Hemorrhages
Splinter hemorrhages sound dramatic, and to be fair, they do look a little dramatic too. These tiny, reddish-brown lines under the nail can make people pause mid-handshake and wonder whether they slammed a finger in a drawer, developed some mysterious deficiency, or accidentally turned their nails into a medical detective story. The truth is more interesting and a lot more practical: splinter hemorrhages are often harmless and caused by everyday trauma, but in some situations they can point to an underlying medical problem that deserves attention.
If you have ever noticed a thin dark streak running in the same direction as your nail growth, you are looking at the classic appearance of a splinter hemorrhage. Most cases are minor and fade as the nail grows out. Still, context matters. One streak after bumping your toe is not the same as repeated streaks across several nails with no obvious cause. That is where symptoms, pattern, and timing become important.
This guide explains what splinter hemorrhages are, what causes them, when they are harmless, when they may signal something more serious, and what treatments actually help. Think of it as a field guide for one of the smallest clues your body can leave in plain sight.
What Are Splinter Hemorrhages?
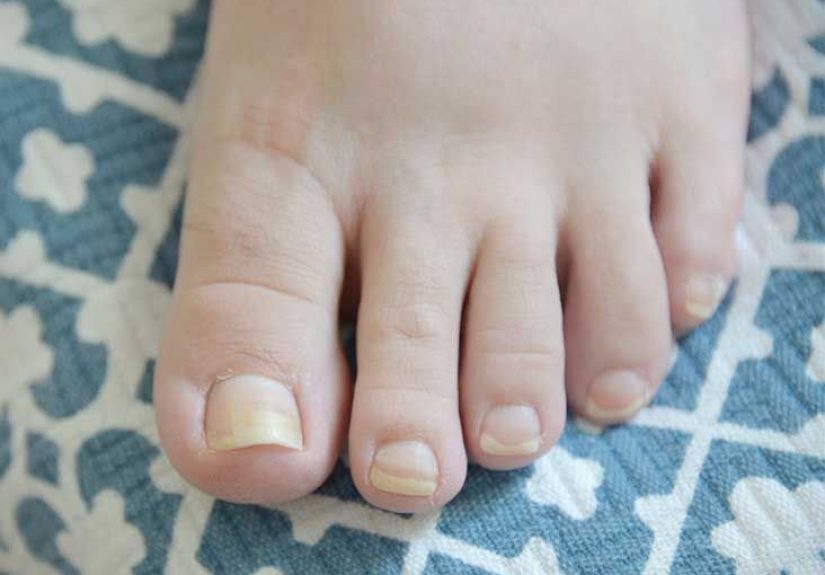
Splinter hemorrhages are tiny areas of bleeding under the fingernails or toenails. They appear as narrow red, reddish-brown, or dark brown lines that run lengthwise, following the direction of nail growth. They get their name because they can look like tiny wood splinters trapped under the nail, except much less rustic and significantly less useful for woodworking.
These streaks form when very small blood vessels in the nail bed become damaged and leak a small amount of blood. The blood gets trapped beneath the nail plate, creating the thin linear mark you can see from above. In many people, this happens after minor injury. In others, the streak can be related to inflammation, infection, vascular disease, or other systemic conditions.
What Do Splinter Hemorrhages Look and Feel Like?
Common symptoms
Splinter hemorrhages usually have a recognizable look. Most people notice:
- Thin vertical lines under the nail
- Red, rust-colored, brown, or dark discoloration
- One or more streaks on a fingernail or toenail
- A mark that does not blanch or disappear when pressed
- Little to no pain unless the nail was recently injured
In trauma-related cases, the streak is often closer to the tip of the nail because that is where repeated impact tends to damage the capillaries. In medical conditions linked to systemic disease, the hemorrhages may appear closer to the base of the nail, affect multiple nails, or recur without a clear reason.
Some people never feel them at all. Others notice tenderness only because the original injury hurt. The hemorrhage itself is usually more of a visual clue than a symptom that causes physical discomfort.
What Causes Splinter Hemorrhages?
There is no single cause, but there is a most common one: trauma. After that, the list gets broader and more medically interesting.
1. Minor trauma and repeated nail stress
This is by far the most common cause. Everyday events can injure the small vessels under the nail, including:
- Stubbing a toe
- Slamming a finger in a door
- Running, hiking, or sports that create repetitive toe impact
- Nail biting or picking
- Aggressive manicures
- Acrylic nails or cosmetic nail procedures
- Repeated friction from shoes, tools, or instruments
When trauma is the cause, the splinter hemorrhage is usually isolated, makes sense in context, and improves as the nail grows.
2. Skin and nail disorders
Several inflammatory conditions can affect the nail unit and trigger these linear bleeds. Nail psoriasis is a well-known example. Psoriasis can also cause pitting, thickening, nail separation, and discoloration, so splinter hemorrhages may show up as part of a larger nail pattern rather than as a random surprise.
Lichen planus and other nail-involving inflammatory disorders can do the same. In these cases, treatment focuses less on the streak itself and more on calming the underlying skin or nail disease.
3. Infections and systemic disease
This is the category that gives splinter hemorrhages their reputation for being medically important. Although they are not common enough to diagnose a serious illness by themselves, they can be one clue in a bigger picture.
One classic association is infective endocarditis, an infection of the heart lining or valves. In that setting, splinter hemorrhages may appear alongside fever, fatigue, chills, shortness of breath, a new or changing heart murmur, or other signs of illness. They are not the most common sign, and they are not present in every case, but they matter because they can contribute to the clinical picture.
Other possible medical associations include:
- Vasculitis
- Connective tissue or autoimmune disorders
- Certain kidney-related conditions
- Systemic infections
- Circulatory or clotting-related problems
Important note: seeing a splinter hemorrhage does not mean someone has a heart infection. It means the pattern has to be interpreted in context, preferably by someone with a stethoscope and a medical license.
4. Medication-related causes
Some medications, especially certain cancer therapies and other drugs that affect blood vessels or the nail bed, have been linked to splinter hemorrhages. If the streaks appear after starting a new medication, especially on several nails at once, it is worth reviewing the timing with a clinician.
When Splinter Hemorrhages Are a Warning Sign
Most splinter hemorrhages are not dangerous. The tricky part is knowing when they are just a harmless souvenir from life and when they deserve a closer look.
You should be more cautious if the splinter hemorrhages:
- Appear on several nails at the same time
- Keep coming back
- Show up without any remembered injury
- Appear closer to the cuticle or proximal nail
- Occur with fever, chills, fatigue, or shortness of breath
- Come with rash, joint pain, or other inflammatory symptoms
- Develop alongside other unusual nail changes
That pattern does not automatically equal a serious diagnosis, but it does shift the conversation from “probably bumped it” to “let’s not ignore this.”
How Doctors Diagnose Splinter Hemorrhages
Diagnosis starts with a basic question that sounds simple but does a lot of heavy lifting: Did you injure the nail? A clinician will usually ask when the streak appeared, whether it is moving with nail growth, whether multiple nails are involved, and whether you have symptoms beyond the nail itself.
The physical exam may include:
- Looking at all fingernails and toenails
- Checking for psoriasis, pitting, or nail separation
- Looking for skin findings such as petechiae, rashes, or lesions
- Listening to the heart if endocarditis is a concern
- Reviewing medications and medical history
If the nail streak looks clearly trauma-related, no elaborate workup may be needed. If the pattern is unexplained or suspicious, testing can include blood work, blood cultures, or an echocardiogram when infection of the heart is being considered. In some cases, dermatology or rheumatology evaluation may help sort out inflammatory or autoimmune causes.
Treatments for Splinter Hemorrhages
The most important treatment principle is refreshingly straightforward: treat the cause, not the streak.
For trauma-related splinter hemorrhages
If the line came from minor injury, the usual treatment is time and patience. The hemorrhage gradually moves outward as the nail grows and eventually disappears. No special cream, miracle oil, or motivational speech for your cuticles is required.
Helpful steps include:
- Protecting the nail from repeated injury
- Wearing shoes that fit properly
- Avoiding picking, biting, or harsh nail grooming
- Giving irritated nails a break from cosmetic procedures
For inflammatory nail disease
If psoriasis or another nail disorder is the culprit, treatment may involve managing the skin disease with topical therapies, injections, or systemic medication depending on severity. The hemorrhage improves when the underlying inflammation is better controlled.
For infection or systemic illness
If a clinician suspects something serious such as infective endocarditis, treatment becomes urgent and focused on the underlying disease. That can involve antibiotics, imaging, specialist care, and close monitoring. In other words, the nail streak is not the main event anymore; it is a clue that helps point to the real problem.
For medication-related cases
When a medication is suspected, the next step is not to stop treatment on your own and stage a one-person rebellion against your prescription list. Instead, a clinician should review the timing, benefits, risks, and whether an adjustment or alternative is appropriate.
How to Protect Your Nails and Lower Your Risk
You cannot prevent every splinter hemorrhage, especially if you are active, athletic, or occasionally meet furniture with your toes at high speed. Still, a few habits can reduce the odds:
- Trim nails neatly without cutting too aggressively
- Wear well-fitting shoes with room for toes
- Use gloves during repetitive hand work
- Be gentle with manicures and nail enhancements
- Avoid biting or picking at nails and cuticles
- Pay attention to repeated or unexplained nail changes
Are Splinter Hemorrhages the Same as a Black Line on the Nail?
No, and this distinction matters. Not every dark or linear nail mark is a splinter hemorrhage. Pigmented nail bands, melanonychia, fungal changes, bruising, and in rare cases subungual melanoma can mimic one another.
A true splinter hemorrhage usually looks like a thin linear bleed and tends to move out with nail growth. A pigmented band may look more solid or uniform. If a dark streak is persistent, changing, unusually wide, irregular, or associated with pigment spreading into the surrounding skin, it needs prompt medical evaluation. That is not the time for internet guessing games.
When to See a Doctor
Make an appointment if you have splinter hemorrhages that are unexplained, recurrent, painful, or appearing on multiple nails. Seek more urgent care if they occur with fever, chills, chest symptoms, severe fatigue, or other signs of systemic illness.
In simple terms, one streak after obvious trauma is usually low drama. Several streaks with no explanation and whole-body symptoms are a different story.
The Bottom Line
Splinter hemorrhages are small linear bleeds under the nail that most often happen after minor trauma. In those everyday cases, they usually go away on their own as the nail grows out. But the pattern matters. Repeated, proximal, or multi-nail hemorrhages, especially with other symptoms, may be a clue to psoriasis, vasculitis, medication effects, or even infective endocarditis.
The good news is that these nail streaks are often more informative than dangerous. Your nails can act like tiny billboards for what is happening in the body. The smart move is not to panic, but not to ignore a suspicious pattern either. When in doubt, let a clinician help decide whether your nail is simply recovering from a bump or waving a small but meaningful red flag.
Real-World Experiences With Splinter Hemorrhages
In real life, splinter hemorrhages rarely show up with a dramatic soundtrack and a spotlight. Most people notice them by accident while typing, washing dishes, scrolling on a phone, or wondering why one toenail suddenly looks like it got into a tiny fight. One of the most common experiences is the athlete or active walker who develops a narrow streak under a toenail after a long run, a hiking weekend, or a stretch of wearing shoes that fit like a bad decision. In that situation, the streak often causes more curiosity than pain. Once the person remembers the extra mileage, the new shoes, or the downhill trail, the mystery starts to solve itself.
Another familiar experience happens with hand-related trauma that barely registers in the moment. Someone works with tools, spends hours gardening, practices guitar, lifts weights, or gets a fresh manicure that was a little too enthusiastic. Days later, a thin brownish line appears under one nail. Because there is no major injury story, the person assumes it came out of nowhere. That is common. Minor nail trauma is easy to forget because the capillaries under the nail do not send a formal written complaint.
Then there are people who notice repeated splinter hemorrhages and start connecting dots. A person with psoriasis may first think they are dealing with cosmetic nail damage, only to realize the nails are also pitted, thickened, or lifting slightly from the nail bed. In these cases, the splinter hemorrhage is less of a solo performance and more of a backup singer in a full nail-psoriasis concert. Once the underlying inflammation is treated, the nail usually becomes less chaotic over time.
The experience is different when splinter hemorrhages appear along with bigger symptoms. Someone may notice streaks on several nails and also feel profoundly tired, feverish, short of breath, or generally unwell. In that context, the nail finding tends to matter because it becomes one visible clue among many. Clinicians often talk about diagnosis as pattern recognition, and this is a perfect example. The streaks alone may not be enough to explain anything, but paired with other symptoms, they can help point attention in the right direction.
There is also the very human emotional side of the experience. Nail changes make people nervous because they are easy to see and hard to interpret. Some assume the worst after a quick internet search. Others dismiss repeated nail findings for months because they feel fine otherwise. Both reactions are understandable. The best real-world lesson is balance: do not panic over one likely trauma-related line, but do not shrug off a recurring or unexplained pattern either.
What many people ultimately learn is that splinter hemorrhages are not really about vanity or cosmetic appearance. They are information. Sometimes that information is simple, like “your hiking boots are too tight.” Sometimes it says, “your psoriasis is more active than you thought.” And sometimes it is the body’s subtle way of asking for a proper medical evaluation. That is what makes splinter hemorrhages worth understanding: they are small, but they are not meaningless.