Table of Contents >> Show >> Hide
- Quick Map: What’s in the Male Reproductive System?
- The Organs, One by One
- Testes (Testicles): The Sperm Factory + Hormone Headquarters
- Scrotum: The Temperature-Controlled “Sperm Storage Bag”
- Epididymis: Sperm’s “Finishing School”
- Vas Deferens: The Delivery Highway
- Seminal Vesicles: The “Sperm Fuel” Mixers
- Prostate Gland: The “Chemistry Lab” for Semen
- Bulbourethral (Cowper’s) Glands: The “Prep Crew”
- Ejaculatory Ducts: The Merge Point
- Urethra: The Shared Exit Lane
- Penis: The Delivery Device
- How It All Works Together
- Puberty, Aging, and What Changes Over Time
- Common Issues and Red Flags
- Keeping the Male Reproductive System Healthy
- Mini FAQ
- Experiences People Commonly Have (A Real-World Look)
- 1) Puberty feels like a surprise group project you didn’t sign up for
- 2) “Is this normal?” is the most popular question on earth
- 3) Doctor visits can feel awkward… but clinicians are not shocked
- 4) Pain and discomfort are where the experience shifts from “awkward” to “important”
- 5) Fertility concerns (for adults) can be unexpectedly emotional
- 6) Confidence often improves with basic knowledge
- Conclusion
- SEO Tags
The male reproductive system is basically a “make, store, and ship” operationexcept the product is sperm, the shipping route is a maze of tiny tubes, and the
quality-control department is run by hormones with strong opinions. If you’ve ever wondered what each organ does, how the whole system works together, and what
changes during puberty and adulthood, you’re in the right place.
This guide breaks down the major male reproductive organs, explains what they do (in plain English), and covers common issueswithout turning your brain into a
biology textbook. Expect real anatomy, real functions, and a few tasteful jokes. (Because if we can’t laugh at how complicated the human body is, what can we
laugh at?)
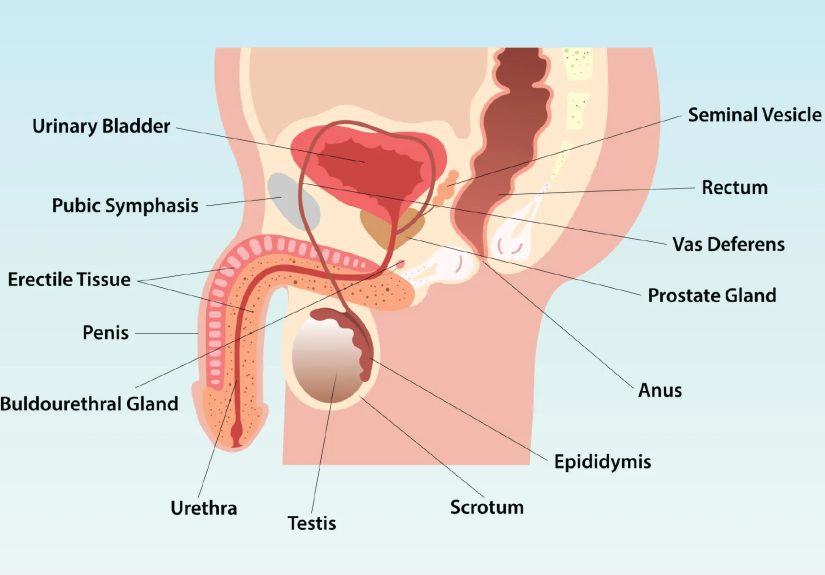
Quick Map: What’s in the Male Reproductive System?
The male reproductive system includes external and internal parts. Some organs are “front-of-house” (outside the body), and others are “back-of-house” (inside
the pelvis). Together, they help:
- Produce sperm (male reproductive cells)
- Produce testosterone and other androgens (sex hormones)
- Move sperm through ducts and mix it with fluids to form semen
- Release semen through the urethra (which is also used for urination)
The Organs, One by One
Testes (Testicles): The Sperm Factory + Hormone Headquarters
The testes are two glands that do two big jobs: (1) make sperm, and (2) make testosterone. Sperm production happens inside tightly coiled tubes called
seminiferous tubules. Testosterone is made by Leydig cells (special cells in the testes). Think of the testes as a factory with
two main product lines: cells (sperm) and chemistry (hormones).
Sperm production isn’t instant. It takes weeks and involves multiple stepskind of like building a car, except the “car” is microscopic and has one mission: deliver
genetic material.
Scrotum: The Temperature-Controlled “Sperm Storage Bag”
The scrotum is a pouch of skin that holds the testes outside the body. Why outside? Because sperm production works best at a slightly cooler temperature than your
body’s core temperature. The scrotum helps regulate that temperature by moving the testes closer to the body when it’s cold and letting them hang farther away when it’s warm.
In other words: your body installed a thermostat… in your pants… for science.
Epididymis: Sperm’s “Finishing School”
Sperm made in the testes aren’t fully ready for action right away. They move into the epididymis, a long, coiled tube on top and behind each testis.
Here, sperm mature and are stored for a while. If the testes are the factory, the epididymis is the quality-control and “final packaging” department.
Vas Deferens: The Delivery Highway
When sperm leaves the epididymis, it travels through the vas deferens (also called the ductus deferens). This is a strong muscular tube that helps
propel sperm forward during ejaculation. The vas deferens travels up into the pelvis and connects into a system of ducts that eventually empties into the urethra.
The vas deferens is also the tube that’s cut or blocked in a vasectomy, which prevents sperm from entering semen.
Seminal Vesicles: The “Sperm Fuel” Mixers
The seminal vesicles are two glands that add fluid to semen. Their secretions contain substances that support sperm, including nutrients (often described as sugar-like
energy sources). This added fluid makes semen volume much larger than sperm alone.
Prostate Gland: The “Chemistry Lab” for Semen
The prostate is a walnut-sized gland below the bladder that surrounds part of the urethra. It contributes fluid to semen and helps with semen’s movement through the
urethra. Prostate fluid is often described as slightly alkaline, which may help sperm function.
Because the prostate hugs the urethra, prostate conditions can affect urinationone reason it gets so much attention in men’s health.
Bulbourethral (Cowper’s) Glands: The “Prep Crew”
These small glands produce a clear, slippery fluid that helps lubricate the urethra and may help neutralize acidity in the urethral pathway. Consider them the
pre-game warmup: not the main event, but helpful for smooth performance.
Ejaculatory Ducts: The Merge Point
The vas deferens and seminal vesicles connect into ducts that pass through the prostate. This is where sperm and gland fluids combine and move toward the urethra.
Urethra: The Shared Exit Lane
The urethra is the tube that carries urine out of the body. In males, it also carries semen out during ejaculation. Importantly, urine and semen don’t come out at
the same timemuscles and valves coordinate the flow like a well-run traffic system (most days).
Penis: The Delivery Device
The penis is the external organ that releases urine and semen through the urethra. It contains specialized erectile tissues (including the corpora cavernosa) that
fill with blood during an erection. Blood flow, nerve signals, and chemical messengers work together to make that happen.
How It All Works Together
Step 1: Hormones Set the Schedule
The male reproductive system is regulated by a hormone “team” that includes the brain and the testes. The hypothalamus releases signals that prompt the pituitary gland
to release LH (luteinizing hormone) and FSH (follicle-stimulating hormone). LH supports testosterone production in Leydig cells,
while FSH supports sperm production within the testes (working with Sertoli cells).
Testosterone then feeds back to the brain to help keep hormone levels in balance. It’s basically a thermostat loopexcept instead of “heat on/heat off,” it’s
“hormones up/hormones down.”
Step 2: Sperm Production Happens in the Testes
Sperm are produced in the seminiferous tubules. This process is called spermatogenesis. It involves cell division, maturation, and a lot of tiny,
carefully timed changes. After sperm form, they move into the epididymis to mature and be stored.
One useful perspective: sperm production is ongoing, not a “batch order.” That’s why overall health and hormone balance can influence sperm quality over time.
Step 3: The Sperm Road Trip (A Very Short Travel Documentary)
Here’s the basic pathway:
- Testes produce sperm
- Epididymis matures and stores sperm
- Vas deferens transports sperm into the pelvis
- Seminal vesicles + prostate add fluids to create semen
- Ejaculatory ducts move semen through the prostate
- Urethra carries semen out through the penis
Along the way, muscles help propel semen during ejaculation. The body coordinates nerves, glands, and smooth muscle contractions like a very fast, very complicated
choreography.
Step 4: Erection Mechanics (A Blood-Flow Story)
An erection depends on a mix of nerve signals and blood flow. One major chemical messenger involved is nitric oxide, which helps relax smooth muscle
in erectile tissue so blood can flow in and be retained. Because erections rely on blood vessels and nerves, ongoing erection problems can sometimes be a sign of
broader health issuesespecially vascular health.
Puberty, Aging, and What Changes Over Time
Puberty: The System Boots Up (With Updates)
During puberty, rising testosterone drives many changes: growth of the testes and penis, increased muscle mass, body hair, voice changes, and the start of regular sperm
production. Puberty timing varies a lotso differences among peers are common and usually normal.
Adulthood: Steady State (Most of the Time)
In adulthood, the system is generally stable, but lifestyle and health factors can influence hormones, sperm quality, and sexual function. Stress, sleep, certain
medications, chronic illness, and substance use can all play a role.
With Age: Fertility Can Change, and the Prostate Gets Opinionated
Testosterone levels may gradually decline with age, and sperm parameters can change too. Many men remain fertile later in life, but the odds of fertility challenges can
rise over time. Prostate enlargement (benign prostatic hyperplasia, or BPH) becomes more common with age and can affect urine flow.
Common Issues and Red Flags
Most of the time, the male reproductive system runs quietly in the background. But some symptoms deserve quick attention.
Seek urgent medical care if you have:
- Sudden, severe testicular pain (especially with swelling or nausea)
- Rapid swelling, redness, or intense tenderness in the scrotum
- Fever with scrotal pain or urinary symptoms
Schedule a medical check if you notice:
- A new lump in a testicle or persistent swelling
- Painful urination or persistent pelvic discomfort
- Blood in urine or semen
- Ongoing trouble getting or maintaining erections
- Concerns about fertility (for adults trying to conceive)
Fertility and Semen Analysis (What It Measures)
A semen analysis looks at semen volume and sperm characteristics like concentration (how many), motility (how they move), and morphology (shape). A single result
doesn’t always tell the whole storyhealth professionals often interpret results alongside medical history and may repeat testing if needed.
Keeping the Male Reproductive System Healthy
- Protect against injury: Use protective gear during contact sports.
- Mind the heat: Prolonged high heat exposure can affect sperm production (relevant mainly for fertility concerns).
- Support overall health: Heart health and metabolic health matter for sexual function because blood flow matters.
- Avoid tobacco and limit substances: These can affect circulation, hormones, and sperm quality.
- Practice safer sex: Using barrier protection and getting tested when appropriate helps reduce STI risk.
- Don’t ignore symptoms: Early evaluation is often simpler than late-stage problem-solving.
Mini FAQ
Is it normal for one testicle to hang lower?
Yes. It’s common for one testicle to sit or hang slightly lower than the other. Bodies are rarely perfectly symmetricalyours included.
Can stress affect sexual function?
Absolutely. Stress can influence hormones, sleep, and nervous system signals. Even without a medical condition, stress can show up as reduced desire or performance issues.
If it persists, it’s worth talking to a healthcare professional.
Does semen always reflect fertility?
Semen analysis is helpful, but it’s not a fortune teller. Results can vary, and “slightly abnormal” results don’t automatically mean infertility. A clinician looks at
the full picture.
Experiences People Commonly Have (A Real-World Look)
Biology is one thing. Living in a body is another. Here are some common experiences people report related to the male reproductive systemespecially during the years
when it’s changing fast.
1) Puberty feels like a surprise group project you didn’t sign up for
Many people describe puberty as a mix of curiosity, awkwardness, and “Why is my body doing this today?” It’s common to notice testicular growth before other changes,
along with new body hair and shifts in sweat and skin oil. Some people experience spontaneous erections, including during sleep. That can feel confusing or embarrassing,
but it’s often a normal part of the nervous system responding to hormones and sleep cycles.
2) “Is this normal?” is the most popular question on earth
Lots of people compare themselves to friends or what they see onlineand that’s where anxiety can sneak in. In reality, bodies vary widely in size, shape, and timing.
One person may start puberty earlier, another later. One person’s voice changes quickly; another’s happens in slow motion. Most of these differences fall within normal.
When a concern is real (like persistent pain, swelling, or a lump), getting checked is a smart movenot an overreaction.
3) Doctor visits can feel awkward… but clinicians are not shocked
Talking about reproductive anatomy can feel personal. Many teens and adults worry they’ll be judged or that their questions are “weird.” In practice, healthcare
professionals discuss these topics constantly. They’re trained to be clinical and respectful. If you’re a teen, it can help to write your questions down ahead of
time, or ask to speak privately for part of the appointment. Many people find that once they start talking, it becomes much easier than expected.
4) Pain and discomfort are where the experience shifts from “awkward” to “important”
People often report that they ignored mild discomfort at first because they didn’t want to bring it up. But certain symptomsespecially sudden, intense testicular pain
are a big deal and should be evaluated quickly. On the other hand, some issues are more common and less urgent (like brief soreness after exercise or minor irritation),
but persistence is the clue: if something lasts, worsens, or repeats, it’s worth checking.
5) Fertility concerns (for adults) can be unexpectedly emotional
When adults start trying to conceive, some are surprised to learn that fertility is not “automatic,” and that male factors can contribute to fertility challenges.
Semen testing can feel personal, even though it’s just a lab assessment of a body system. Many people describe a mix of relief (finally getting information) and stress
(wondering what it means). The healthiest mindset is often the most practical one: a semen analysis is data, not a verdict. Clinicians frequently repeat tests, look for
treatable causes, and consider the couple’s overall situation.
6) Confidence often improves with basic knowledge
A consistent theme: learning anatomy reduces anxiety. Once people understand the pathway of sperm, the role of hormones, and what symptoms matter, they feel more in
control. That doesn’t mean overanalyzing every sensation. It means knowing what’s normal, what’s variable, and what’s worth bringing up with a professional.
Bottom line: the male reproductive system is normal to talk about, normal to learn about, and normal to ask questions about. Your body isn’t “weird”it’s human.
And humans are famously complicated.
Conclusion
The male reproductive system is a coordinated network of organs and hormones designed to produce sperm, create semen, and support sexual functionwhile sharing space
(and plumbing) with the urinary system. When you understand what each organ doestestes for sperm and testosterone, epididymis for maturation, vas deferens for
transport, glands for semen fluid, urethra for exitit becomes much easier to understand what’s normal, what changes with age, and when symptoms may signal a problem.
If something feels offpain, swelling, lumps, urinary changes, or persistent sexual function concernsgetting medical advice early is the smartest move. Not because
everything is an emergency, but because your body is worth taking seriously.







