Table of Contents >> Show >> Hide
Warts are the skin’s version of an uninvited party guest: common, clingy, and rarely dangerous, but definitely not something most people are thrilled to host. The good news is that most warts are harmless, many eventually leave on their own, and several treatments can speed up the breakup.
If you have ever stared at a weird bump on your finger, foot, face, or somewhere more private and wondered, “Is this a wart, and why is it so committed to staying?” this guide has you covered. Below, we break down the main types of warts, what causes them, how they tend to look in photos and real life, the best treatment options, and the smart moments to stop Googling and call a doctor.
What Are Warts?
Warts are small, noncancerous growths caused by certain types of human papillomavirus, better known as HPV. The virus infects the outer layer of skin, often through tiny cuts, hangnails, shaving nicks, or other weak spots. Once it settles in, the skin starts growing in a rough, thickened, or bumpy way, and voilà: wart.
Most skin warts are benign and are not the same thing as cancer. Common skin warts on the hands and feet usually come from cutaneous HPV types, which are different from the HPV types linked to genital warts and certain cancers. That distinction matters, because “wart” is one word doing a lot of work.
Warts are contagious, but not dramatically so. You can catch the virus through direct skin contact or from shared personal items such as towels, razors, pumice stones, socks, or nail tools. Even then, not everyone exposed to HPV develops a wart. Your immune system gets a vote.
Types of Warts
Common warts
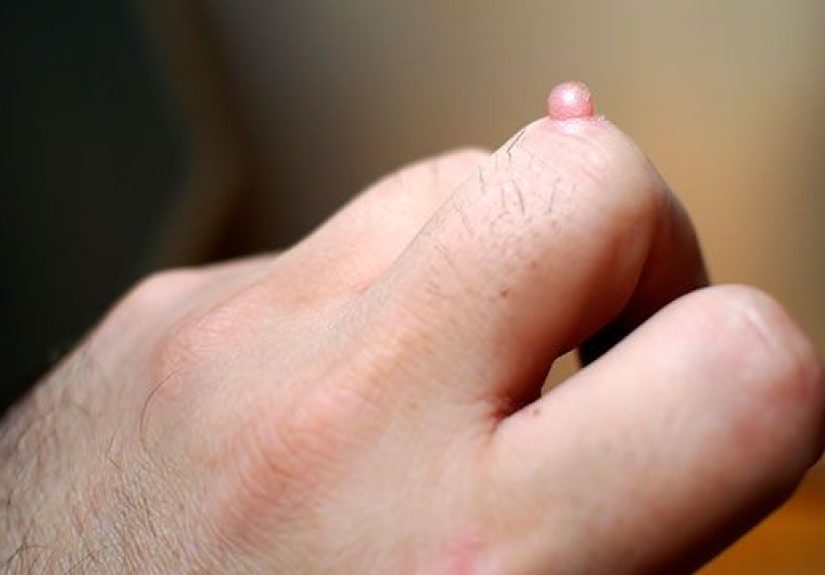
Common warts are the classic version most people picture. They usually appear on the fingers, around the nails, the backs of the hands, elbows, or knees. They tend to be round or oval with a rough surface and may contain black pinpoint dots, which are tiny blood vessels, not actual seeds. In other words, the wart is weird enough already; it does not need botanical drama.
Plantar warts
Plantar warts grow on the soles of the feet, especially the heel, ball of the foot, or base of the toes. Because body weight presses them inward, they can look flatter than other warts and may be covered by thick callused skin. They are often tender when walking or standing, and they can interrupt the normal skin lines on the bottom of the foot.
Mosaic warts
Mosaic warts are clusters of plantar warts that merge together and cover a wider area. They can be stubborn, uncomfortable, and annoying in that special way only foot problems can be.
Flat warts
Flat warts are smaller and smoother than common warts. They often appear in clusters and are common on the face, forehead, neck, legs, or beard area. In children, they often show up on the face. In adults, they can spread in areas that are shaved, because shaving can move the virus around like an unhelpful delivery service.
Filiform warts
Filiform warts look thread-like or finger-like rather than round. They often develop quickly on the face, especially around the mouth, eyes, or nose. They can be skin-colored, pink, yellow, white, gray, or brown, depending on skin tone and lighting.
Periungual and subungual warts
These warts grow around or under the fingernails and toenails. They can distort nail growth, become painful, and be especially tough to treat. If you bite your nails or pick at cuticles, the virus gets an open invitation.
Genital warts
Genital warts are caused by different HPV types and are spread through sexual contact. They may be small, flesh-colored, pink, gray, or brown, and can appear as smooth bumps or cauliflower-like clusters. They require a different treatment approach than common skin warts, so over-the-counter wart remover is not the hero here.
What Warts Look Like in Images
If you are comparing your skin bump to photos online, here are the most useful visual clues:
- Common wart: rough, raised bump on fingers or hands, sometimes with black dots.
- Plantar wart: thickened spot on the sole with black pinpoints and pain under pressure.
- Mosaic wart: multiple plantar warts grouped into a patch.
- Flat wart: many tiny, smooth, flat-topped bumps on the face or shaved areas.
- Filiform wart: narrow, thread-like projection, often near the mouth, nose, or eyelids.
- Genital wart: soft bumps or clustered growths in the genital or anal area.
One important warning: not every wart-looking bump is a wart. Seborrheic keratoses, calluses, skin tags, and even some skin cancers can mimic warts. If a growth is changing, bleeding, very painful, oddly pigmented, or just suspicious-looking, skip the home chemistry set and get it checked.
What Causes Warts?
The direct cause is HPV infection in the skin. But the bigger story is how the virus gets in. Tiny breaks in the skin act like a side door. That is why warts often show up near hangnails, around bitten nails, on shaved skin, or on pressure points of the feet.
Risk factors include being a child or teen, having a weakened immune system, biting nails, picking at skin, shaving over an existing wart, and walking barefoot in shared damp areas like locker rooms or pool decks. Warts are also more likely to spread when people share towels, razors, socks, nail clippers, or pumice stones.
Still, HPV is extremely common, so getting a wart does not mean you did anything wrong. Sometimes it just means your immune system and a tiny skin break had a brief lapse in judgment.
Do Warts Go Away on Their Own?
Often, yes. Many warts disappear without treatment as the immune system gradually recognizes the virus and clears the infected skin. But “eventually” can mean months, and sometimes a year or two. Plantar warts and periungual warts tend to be more stubborn. In kids, warts often clear faster than they do in adults, although “faster” is still not always fast enough to make anyone happy.
That is why treatment is usually about one of three goals: speeding up clearance, relieving pain, or avoiding spread. Cosmetic frustration also counts. Human beings are allowed to be annoyed by weird bumps.
Wart Treatment Options
Salicylic acid
This is one of the most common and best-studied over-the-counter treatments for ordinary skin warts. It works by gradually peeling away layers of the wart. It comes as liquids, gels, pads, and medicated tapes. Consistency matters a lot. You usually need daily treatment for weeks, sometimes longer, plus occasional gentle filing of dead skin after soaking.
Do not use salicylic acid on the face or genital area. Use extra caution if you have diabetes, poor circulation, or nerve problems, and ask a clinician first.
At-home freezing products
Drugstore freezing kits can help with some small warts, though they are not as strong as the liquid nitrogen used in a medical office. They can be worth trying for uncomplicated warts on the hands or feet, but results vary.
Duct tape
Yes, duct tape continues its side quest as a folk remedy. Dermatologists sometimes suggest it as part of a home routine because it may irritate the skin enough to wake up the immune system and can also help soften thickened skin. It is not magic, but it is cheap and oddly confident.
Cryotherapy in a clinic
In-office freezing with liquid nitrogen is a common treatment for stubborn warts. It is stronger than home products and often works better, though it may require repeated sessions. It can sting, blister, and temporarily discolor the skin.
Prescription treatments
Doctors may prescribe stronger peeling agents, blistering solutions, 5-fluorouracil, imiquimod, or other topical medications depending on the wart type and location. Some of these are used more often for flat warts, difficult plantar warts, or genital warts.
Immunotherapy
For stubborn cases, dermatologists sometimes use treatments designed to get the immune system to fight the wart more effectively. That may include injected or topical therapies. This approach is especially useful when ordinary freezing and peeling are not getting the job done.
Electrosurgery, laser therapy, and excision
These office procedures are usually reserved for difficult or persistent warts. They can work well, but they may involve discomfort, recovery time, and a risk of scarring. Translation: useful tools, just not always first-date material.
Genital wart treatment
Genital warts are treated differently from common skin warts. A clinician may use prescription creams or ointments, cryotherapy, electrocautery, chemical treatments, or removal procedures. Even when visible warts are removed, HPV can remain in the body, and warts can recur.
When to See a Doctor
You should get medical advice if:
- the wart is on your face, genitals, or inside the mouth, vagina, or anus;
- it hurts, burns, bleeds, changes color, or changes shape;
- you are not sure it is actually a wart;
- you have many warts or they keep spreading;
- you tried home treatment and it is not working;
- you have diabetes, poor circulation, neuropathy, or a weakened immune system.
Also, please do not cut, burn, rip, or carve out a wart at home. That is not self-care. That is a future infection with a plot twist.
Can Warts Be Prevented?
You cannot reduce the risk to zero, because HPV is common and widespread. But you can improve the odds:
- Do not touch or pick at warts.
- Wash your hands after treating a wart.
- Do not share towels, razors, socks, pumice stones, or nail tools.
- Keep cuts and scrapes clean and covered.
- Wear flip-flops in locker rooms, pool areas, and communal showers.
- Avoid shaving over a wart.
- Keep feet dry and wear shoes that fit well.
For genital warts, prevention also includes safer sex practices and HPV vaccination. The HPV vaccine is recommended routinely at age 11 or 12 and can be started at age 9. It helps prevent genital warts caused by HPV types 6 and 11, along with many HPV-related cancers. It does not treat an existing wart, but it is excellent prevention.
Quick FAQs
Are warts contagious?
Yes. They can spread to other people and to other areas of your own body.
Are all warts caused by the same HPV?
No. HPV is a large family of viruses. Different types are linked to different kinds of warts and different health risks.
Do common warts mean cancer risk?
No. Common skin warts on the hands and feet are usually caused by cutaneous HPV types that do not cause genital warts or cancer.
What is the fastest way to get rid of a wart?
For rapid removal, a dermatologist is usually your best bet. In-office treatment tends to work faster than home treatment, especially for painful or stubborn warts.
Can I treat every wart at home?
No. Do not self-treat warts on the face or genitals, and do not treat any bump you are not sure is a wart.
Real-Life Wart Experiences and What They Teach Us
The following are composite, realistic experiences based on common clinical patterns and patient complaints, not single identified case histories. They show how warts affect daily life far beyond “just a small bump.”
The middle-school finger wart. A 12-year-old notices a rough bump near the nail of the index finger. At first it is ignored because, honestly, homework is already enough trouble. A few weeks later, there are two bumps. Then three. Nail biting and picking at the area help spread the virus, and suddenly what looked minor becomes a little cluster around the nail fold. The lesson here is simple: warts often spread when irritated, and hands are high-traffic real estate.
The runner with a plantar wart. An adult training for a 10K starts feeling like there is a pebble stuck in one shoe. It turns out to be a plantar wart hidden under a thick callus. Because these warts get pushed inward, they can be less obvious to the eye than they are to the nerves. Walking hurts, standing hurts, and exercise becomes a negotiation. Many people in this situation wait too long, assuming it is “just a callus,” when earlier treatment could have reduced pain faster.
The shaving-related flat wart surprise. Someone notices tiny smooth bumps along the jawline or legs and assumes it is acne, razor burn, or irritation. But flat warts can spread in shaved areas, and repeated shaving can create a whole collection where there used to be one or two. This is one reason “just keep exfoliating” is not a universal skin-care strategy. Sometimes the issue is viral, not cosmetic.
The embarrassment factor. A lot of people are less bothered by physical pain than by the social weirdness of having a visible wart. A wart on the hand can lead to hiding fingers in photos, avoiding handshakes, or feeling self-conscious during work and school. Genital warts can create even more anxiety, because they bring up worries about sex, relationships, stigma, recurrence, and cancer risk. Good medical counseling matters here. Patients need facts, not panic. The right treatment plan can help, but reassurance is also treatment.
The stubborn wart that refuses to resign. One of the most frustrating experiences is the wart that seems to disappear, only to come back like it forgot its keys. This happens because the visible thick skin may improve before the infected tissue at the base is fully cleared. Inconsistent treatment is a big reason warts linger. Many people quit salicylic acid too soon, stop freezing after one round, or forget daily care once the wart looks flatter. Warts reward persistence more than enthusiasm.
The immunocompromised patient. For people with weakened immune systems, warts can be more numerous, more stubborn, and more likely to recur. This changes the treatment conversation. What might be a simple over-the-counter problem for one person can become a long-term dermatology issue for another. It is a useful reminder that skin is not separate from the rest of health. The immune system is part of the story every time.
Put all these experiences together, and one message becomes clear: warts may be common, but they are not always trivial. They can interfere with sports, confidence, comfort, grooming, and everyday routines. The most effective approach is usually a combination of correct identification, patience, consistent treatment, and medical help when the wart is painful, spreading, or suspicious.
Conclusion
Warts are common, contagious, and usually harmless, but they come in several forms and do not all behave the same way. Common warts, plantar warts, flat warts, filiform warts, periungual warts, and genital warts each have their own favorite location, look, and treatment strategy. Many eventually fade on their own, but salicylic acid, cryotherapy, prescription therapies, and dermatologist procedures can help clear them faster. And when a bump looks unusual, hurts, bleeds, or appears on the face or genitals, it is smart to get a professional opinion instead of declaring war with a nail clipper.






