Table of Contents >> Show >> Hide
- What Is Knee Arthroscopy?
- How Knee Arthroscopy Works
- When Arthroscopy for Knee Pain May Help
- When Knee Arthroscopy Is Usually Not Recommended
- Benefits of Arthroscopic Knee Surgery
- Risks and Possible Complications
- Recovery After Knee Arthroscopy
- Alternatives to Arthroscopy for Knee Pain
- Questions to Ask Before Knee Arthroscopy
- Real-Life Experiences: What Patients Often Learn About Arthroscopy for Knee Pain
- Conclusion
Arthroscopy for knee pain can sound like the orthopedic version of sending a tiny detective into your joint with a flashlight. In a way, that is not far off. During knee arthroscopy, a surgeon inserts a small camera through tiny incisions to look inside the knee and, when appropriate, treat certain problems such as meniscus tears, loose cartilage fragments, ligament injuries, or inflamed tissue.
But here is the plot twist: knee arthroscopy is not a magic eraser for every aching knee. It can be useful in the right situation, yet research has shown that it is often not helpful for routine osteoarthritis pain or general age-related wear and tear. The key is knowing when arthroscopic knee surgery makes sense, when conservative care may be smarter, and what recovery really looks like after the “tiny camera adventure” is over.
What Is Knee Arthroscopy?
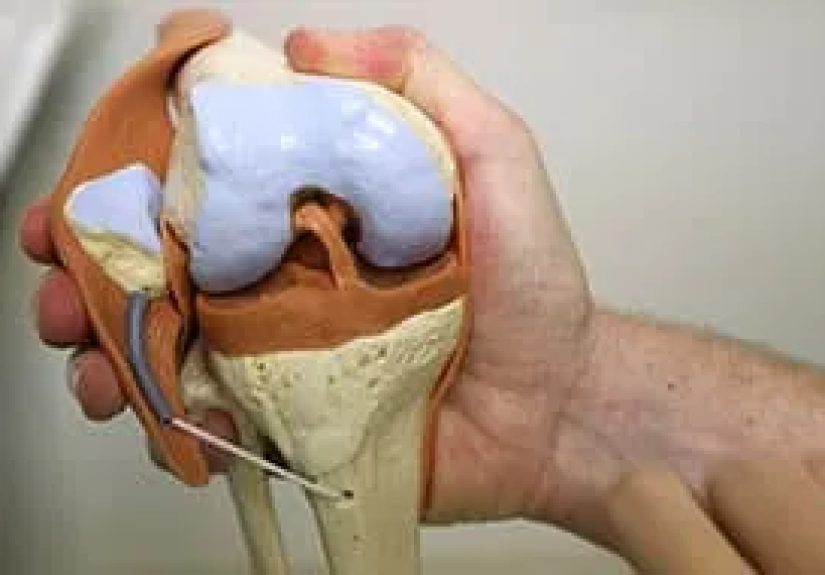
Knee arthroscopy is a minimally invasive surgical procedure used to diagnose and treat certain conditions inside the knee joint. Instead of making one large incision, the surgeon makes a few small openings around the knee. Through one opening, the surgeon inserts an arthroscope, a narrow instrument with a camera and light. Through other small openings, miniature surgical tools may be used to repair, trim, remove, or smooth damaged tissue.
Compared with open knee surgery, arthroscopy usually involves smaller incisions, less soft-tissue disruption, and a faster early recovery. Many procedures are done on an outpatient basis, meaning the patient goes home the same day. That said, “minimally invasive” does not mean “minor enough to ignore.” It is still surgery, with anesthesia, recovery time, rehabilitation, and possible complications.
Common knee problems evaluated or treated with arthroscopy
Doctors may consider knee arthroscopy for problems such as a torn meniscus, loose bodies in the joint, cartilage injuries, certain kneecap tracking issues, synovial inflammation, or ligament-related conditions. In some cases, arthroscopy is used when imaging and physical exams do not fully explain symptoms. More often, it is used when the diagnosis is already clear and the surgeon believes a specific mechanical problem can be treated.
How Knee Arthroscopy Works
Before surgery, the medical team reviews symptoms, medical history, imaging results, medications, allergies, and anesthesia risks. Patients are usually told when to stop eating or drinking before the procedure and whether to pause certain medications. Because anesthesia and pain medicine can affect alertness, patients typically need someone to drive them home.
During the procedure, the knee is cleaned and prepared. The surgeon fills the joint with sterile fluid, which helps expand the space inside the knee and improves visibility. The arthroscope sends images to a monitor, allowing the surgeon to inspect cartilage, ligaments, the meniscus, and other structures. If treatment is needed, small instruments can be inserted to repair a tear, remove loose fragments, trim damaged tissue, or address other targeted issues.
The incisions are then closed, the knee is bandaged, and the patient is moved to recovery. Some patients are allowed to bear weight quickly, while others need crutches, a brace, or limited movement depending on what was done inside the joint. A simple diagnostic arthroscopy is very different from a meniscus repair or ligament reconstruction, so recovery instructions should always be personalized.
When Arthroscopy for Knee Pain May Help
The best candidates for arthroscopy usually have a clear structural problem that matches their symptoms. For example, a younger athlete with a traumatic meniscus tear after twisting the knee during sports may be very different from an older adult with gradual knee pain, arthritis changes on X-ray, and a degenerative meniscus tear found on MRI.
Mechanical symptoms matter
Arthroscopy may be more reasonable when a person has true mechanical symptoms, such as the knee locking and not fully straightening, catching in a way that limits movement, or swelling after a specific injury. A loose fragment of cartilage or bone floating inside the joint can sometimes act like a pebble in a door hinge. In that case, removing the fragment may improve movement and comfort.
Traumatic meniscus tears
The meniscus is a C-shaped shock absorber between the thighbone and shinbone. A sudden twist can tear it, especially during sports, squatting, pivoting, or awkward landings. Some meniscus tears can be repaired, especially if the tear is in an area with better blood supply. Others may require trimming of the unstable portion. The goal is to preserve as much healthy meniscus as possible because the meniscus helps protect the knee from future arthritis.
Loose bodies and cartilage fragments
Loose bodies may develop after injury, cartilage damage, or certain joint conditions. These fragments can cause catching, swelling, or sudden sharp pain. Arthroscopy may help remove them and improve joint motion. However, if the entire joint is affected by advanced osteoarthritis, removing a fragment may not solve the bigger pain problem.
When Knee Arthroscopy Is Usually Not Recommended
This is where modern evidence gets serious. Arthroscopy is generally not recommended as a routine treatment for knee osteoarthritis, degenerative knee disease, or vague chronic knee pain without a clear mechanical target. Many studies have found that arthroscopic procedures such as lavage, debridement, or partial meniscectomy often do not provide meaningful long-term improvement for degenerative knee pain compared with non-surgical care.
That can be frustrating for patients because knee pain is real, annoying, and sometimes life-limiting. But if the pain is mainly from arthritis, inflammation, reduced cartilage, muscle weakness, excess joint load, or widespread degenerative change, a scope may not address the root cause. It is a bit like vacuuming one corner of a room when the whole roof is leaking. Technically, something was done, but the main problem remains.
Degenerative meniscus tears are tricky
Degenerative meniscus tears are common as people age. In fact, imaging can show meniscus tears in people who have little or no knee pain. That means the tear may not be the main pain generator. Treating the MRI finding instead of the patient’s actual symptoms can lead to disappointment, extra cost, and recovery time without a clear benefit.
Osteoarthritis needs a broader plan
For osteoarthritis-related knee pain, treatment usually focuses on exercise therapy, weight management when appropriate, low-impact activity, anti-inflammatory strategies, bracing, physical therapy, injections in selected cases, and eventually joint replacement for severe disease. Arthroscopy rarely changes the long-term course of arthritis.
Benefits of Arthroscopic Knee Surgery
When arthroscopy is used for the right reason, it can offer several benefits. Small incisions may mean less early pain than open surgery, and many patients can return home the same day. Surgeons can view the inside of the knee directly and treat targeted problems with precision. For certain injuries, arthroscopy can help restore motion, reduce catching, and support a return to activity.
Another advantage is diagnostic clarity. MRI is useful, but it is not perfect. Arthroscopy allows the surgeon to see the joint directly. However, because arthroscopy is invasive, it is usually not the first diagnostic step. Most knee pain can be evaluated with a history, physical exam, X-rays, and sometimes MRI before surgery is even discussed.
Risks and Possible Complications
Knee arthroscopy is generally considered safe, but every surgery has risks. Possible complications include infection, bleeding, blood clots, nerve or blood vessel injury, stiffness, ongoing swelling, anesthesia problems, and persistent knee pain. Some patients feel better quickly, while others discover that the knee still complains like a tiny sports commentator after every staircase.
Blood clots are uncommon but important. Warning signs may include calf swelling, unusual warmth, worsening leg pain, chest pain, or shortness of breath. Infection warning signs may include fever, increasing redness, drainage, or worsening pain around the incision. Patients should follow their surgeon’s instructions and seek medical care promptly if concerning symptoms appear.
The risk of continued pain
One of the most overlooked risks is not dramatic but deeply frustrating: the surgery may not relieve the pain. This is especially true when pain comes from arthritis, widespread cartilage loss, or non-mechanical causes. A technically successful arthroscopy can still leave a patient unhappy if expectations were unrealistic.
Recovery After Knee Arthroscopy
Recovery depends on the procedure. A simple meniscus trim may allow faster walking and a shorter recovery than a meniscus repair, which often requires more protection because the tissue needs time to heal. Ligament reconstruction or cartilage restoration can involve months of structured rehabilitation.
In the first few days, patients are often advised to elevate the leg, use ice as directed, keep the incision clean and dry, take prescribed medications safely, and perform gentle exercises recommended by the care team. Crutches may be used to reduce pressure on the knee. Physical therapy often focuses first on swelling control, range of motion, and activating the quadriceps muscle, which loves to go on vacation after knee surgery.
Typical recovery milestones
Many people return to desk work within a few days to two weeks after simpler procedures, depending on pain, swelling, mobility, and transportation needs. Jobs that require standing, climbing, kneeling, or lifting may require more time. Return to sports may take weeks to months, and after meniscus repair or ligament reconstruction, the timeline can be significantly longer.
The best recovery is not about rushing. It is about gradually restoring motion, strength, balance, and confidence. Doing too much too soon can increase swelling and delay progress. Doing too little can lead to stiffness and weakness. The sweet spot is guided progression, preferably with a physical therapist or a detailed rehab plan from the surgeon.
Alternatives to Arthroscopy for Knee Pain
Before choosing surgery, many people benefit from a strong non-surgical plan. Conservative care is not “doing nothing.” It is active treatment, and for many types of knee pain, it works surprisingly well.
Physical therapy
Physical therapy can strengthen the quadriceps, hamstrings, glutes, and hip stabilizers. Stronger muscles help control knee movement and reduce stress on irritated structures. Therapy may also improve flexibility, walking mechanics, balance, and confidence with stairs or squats.
Low-impact exercise
Walking, cycling, swimming, and elliptical training can help keep the knee moving without pounding it like a drum solo. Movement supports joint nutrition, reduces stiffness, and helps maintain overall health. The trick is choosing activities that challenge the body without causing major pain flares.
Weight management and load reduction
For people carrying extra body weight, even modest weight loss can reduce stress across the knee joint. Assistive devices, supportive shoes, activity pacing, and braces may also help. The goal is not to become a fitness influencer overnight. The goal is to make the knee’s daily workload more reasonable.
Medication and injections
Doctors may recommend topical anti-inflammatory gels, oral pain relievers, anti-inflammatory medicines, or injections depending on the diagnosis and medical history. These options should be discussed with a healthcare professional, especially for people with stomach, kidney, heart, bleeding, or medication-interaction concerns.
Questions to Ask Before Knee Arthroscopy
Before agreeing to arthroscopic knee surgery, patients should feel comfortable asking direct questions. A good surgeon will not be offended. In fact, clear questions make the decision smarter.
- What exact problem are you trying to fix with arthroscopy?
- Does my pain match the MRI finding?
- Do I have osteoarthritis, and how does that affect the expected result?
- What are my non-surgical options?
- What happens if I wait and try physical therapy first?
- Will you repair tissue, trim tissue, remove loose bodies, or only inspect the joint?
- How long will I need crutches, a brace, or physical therapy?
- What results are realistic for someone with my age, activity level, and diagnosis?
The most important question may be this: “What is the goal of surgery?” If the answer is specific, measurable, and tied to a clear structural problem, arthroscopy may be worth discussing. If the answer is vague, it may be time for a second opinion.
Real-Life Experiences: What Patients Often Learn About Arthroscopy for Knee Pain
Many people go into knee arthroscopy expecting a quick fix. After all, the incisions are small, the camera is tiny, and the phrase “outpatient procedure” sounds almost casual. But patient experiences vary widely. Some people feel relief because the surgery addressed a specific problem, such as a flap of torn meniscus catching in the joint. Others recover from the procedure only to realize their original pain was mostly from arthritis, muscle weakness, or inflammation that surgery could not fully solve.
One common experience is the surprise of post-surgery swelling. A patient may look at the small bandages and think, “Great, tiny holes, tiny problem.” Then the knee swells after walking too much, and reality enters the room carrying an ice pack. Swelling does not always mean something is wrong. It can be part of normal healing, especially after activity. But it is a signal to slow down, elevate, ice if recommended, and follow the rehab plan.
Another common lesson is that the quadriceps muscle can become sleepy after knee surgery. Even active people may struggle to fully straighten the knee or lift the leg at first. This is why early exercises are often simple: ankle pumps, quad sets, heel slides, and straight-leg raises when cleared. They may not look impressive on social media, but they are the foundation. Rehab is not always glamorous. Sometimes victory is bending the knee a few more degrees without making a face.
Patients who do best often treat recovery as a process, not a race. They attend physical therapy, ask questions, track swelling, and build activity gradually. They do not test the knee every hour like it is a new phone feature. They respect pain signals and understand the difference between normal soreness and worsening symptoms. They also keep expectations realistic. Arthroscopy can improve mechanical symptoms, but it does not make a 55-year-old arthritic knee behave like a brand-new knee fresh from the factory.
People who feel disappointed after arthroscopy often describe a mismatch between expectations and the actual diagnosis. For example, someone with moderate osteoarthritis and a degenerative meniscus tear may expect the surgery to “clean out the knee” and remove pain. But if the joint surfaces are already worn and irritated, trimming a meniscus tear may not change the larger biology of the knee. This is why shared decision-making matters so much before surgery.
Another experience worth mentioning is the emotional side. Knee pain affects sleep, work, exercise, and mood. When walking the dog or climbing stairs becomes a negotiation, people understandably want a solution. Surgery can feel like decisive action. But sometimes the bravest and smartest choice is a committed non-surgical plan first: physical therapy, strength training, low-impact exercise, weight management if needed, and careful symptom tracking. Conservative care may sound less dramatic, but it can be powerful.
For patients who truly need arthroscopy, preparation helps. Arrange transportation, set up a comfortable recovery area, place essentials within reach, prepare easy meals, and clarify medication instructions. Ask when to shower, when to change bandages, when to start exercises, and which symptoms require a call. The smoother the first week, the less likely recovery will feel like a confusing obstacle course designed by someone who hates knees.
The biggest takeaway from real-world experiences is simple: knee arthroscopy is a tool, not a universal cure. In the right patient, for the right problem, it can be very helpful. In the wrong situation, it can add recovery time without solving the main pain source. A good decision begins with a clear diagnosis, honest expectations, and a plan that treats the whole kneenot just the part that looked suspicious on an MRI.
Conclusion
Arthroscopy for knee pain can be valuable when there is a specific mechanical problem, such as a repairable meniscus tear, a loose body, or a structural injury that matches the patient’s symptoms. However, it is usually not the best answer for routine osteoarthritis pain or degenerative knee disease. The most successful decisions come from matching the treatment to the true cause of pain.
If you are considering arthroscopic knee surgery, ask what the surgeon expects to fix, what results are realistic, and whether non-surgical care should be tried first. A tiny camera can see inside the knee, but good decision-making requires the bigger picture: your symptoms, imaging, activity goals, arthritis level, health history, and recovery commitment.
Note: This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment from a qualified healthcare professional. Anyone with knee pain, swelling, locking, injury, or worsening symptoms should consult a licensed medical provider.