Table of Contents >> Show >> Hide
- Why So Many Serious Illnesses Get Mistaken for the Flu
- The Conditions Most Likely To Turn a “Probably Viral” Visit Into a Bigger Story
- 1. Sepsis: The Fast Escalator Nobody Wants
- 2. Meningitis: When a “Bad Bug” Is Much More Than a Bug
- 3. Appendicitis: The “Stomach Flu” Impostor
- 4. Pneumonia: The Flu’s Meaner Cousin
- 5. Pulmonary Embolism: The Silent Ambush
- 6. Heart Attack: Not Always the Hollywood Version
- 7. Stroke: The One That Does Not Wait for Convenience
- Why Misdiagnosis Stories Spread So Fast Online
- Red Flags That Deserve Faster Medical Attention
- How To Advocate for Yourself Without Turning Into Your Own Doom Blogger
- The Big Lesson Behind the Wildest Misdiagnosis Stories
- Experiences People Keep Sharing About “Flu Or Fatal” Mix-Ups
At first, it sounds like a very ordinary bad week: a fever, body aches, exhaustion, maybe a cough, maybe some nausea, maybe a dramatic declaration that “this flu is trying to end me.” Then the plot twists. It is not the flu. It is meningitis. Or sepsis. Or appendicitis. Or pneumonia. Or a heart attack wearing a discount Halloween mask and pretending to be a stomach bug.
That is why stories about misdiagnosis hit such a nerve online. People share them because they are scary, messy, and deeply relatable. Most of us have been told to rest, hydrate, and wait it out. Usually, that is perfectly reasonable advice. But sometimes a dangerous condition shows up in a flimsy disguise, borrowing the same vague symptoms as influenza or a “virus going around.” That overlap is where things get complicated, and sometimes where things go very wrong.
This article is not here to turn every sniffle into a five-alarm emergency. Nobody needs a panic attack every time they get chills in January. But it is worth understanding why some illnesses are missed, why “flu-like symptoms” can be a diagnostic trap, and which warning signs deserve faster action. Because the difference between a routine viral illness and a medical emergency is not always obvious on day one.
Why So Many Serious Illnesses Get Mistaken for the Flu
The flu is a symptom copycat magnet. Real influenza can cause fever, chills, headache, muscle aches, fatigue, cough, sore throat, and a general feeling that your body has filed a formal complaint against you. The problem is that many other conditions can open with the same vague misery.
Early in an illness, doctors and patients are often working with incomplete information. Symptoms may still be evolving. A cough has not fully arrived yet. The abdominal pain has not localized. The stiff neck is not obvious. The shortness of breath is still mild enough that someone says, “I’m fine, I’m just tired.” In medicine, timing matters. A disease seen too early can look like something much simpler.
There is also a very human tendency to choose the most common explanation first. During respiratory virus season, “it’s probably the flu” can sound logical. Usually, it is. But common things being common does not mean dangerous things stop existing. The body, annoyingly, does not always respect neat diagnostic categories.
Another issue is that serious conditions often have atypical symptoms. A heart attack does not always arrive with movie-style chest clutching. Appendicitis does not always read the textbook before making an entrance. Sepsis can begin subtly. Meningitis may start like “the worst flu of my life” before it becomes unmistakably worse. When symptoms do not follow the classic script, both patients and clinicians can get thrown off.
The Conditions Most Likely To Turn a “Probably Viral” Visit Into a Bigger Story
1. Sepsis: The Fast Escalator Nobody Wants
Sepsis is one of the biggest reasons “I thought it was just the flu” stories become frightening. It is the body’s extreme, dangerous response to an infection. The underlying infection might begin in the lungs, urinary tract, skin, or somewhere else entirely. At first, a person may have fever, chills, weakness, confusion, nausea, rapid breathing, or just an overwhelming sense that something is very wrong. That overlap with flu symptoms is part of what makes it so easy to underestimate.
What changes the tone is speed. Sepsis can worsen fast. The person who was miserable in the morning may be disoriented, short of breath, or unusually weak by evening. That “crashed out of nowhere” feeling appears again and again in patient stories. In reality, it usually did not come out of nowhere. It was building while everyone, understandably, hoped it was a nasty virus.
2. Meningitis: When a “Bad Bug” Is Much More Than a Bug
Meningitis often starts with symptoms nobody would frame and put on a diagnostic trophy shelf: fever, headache, nausea, fatigue. That is exactly why it can be missed early. Later, red flags such as a stiff neck, confusion, sensitivity to light, severe headache, sleepiness, or seizures can make the picture clearer. But early on, it may sound like flu, COVID, or a brutal viral infection.
This is where many online misdiagnosis stories get their emotional punch. Someone says they were told to rest, take over-the-counter meds, and come back if needed. Then the symptoms escalate in a way that feels sudden and surreal. The lesson is not “never trust an initial diagnosis.” The lesson is that change matters. A diagnosis should be allowed to evolve when the illness does.
3. Appendicitis: The “Stomach Flu” Impostor
Appendicitis has fooled plenty of people because it can begin with nausea, vomiting, low-grade fever, and general belly misery. In the beginning, it may feel like food poisoning, a stomach virus, or a regrettable decision involving gas-station sushi. But the classic warning sign is abdominal pain that worsens, often becoming more focused on the lower right side.
The catch is that not everyone presents classically. Children, older adults, pregnant patients, and people with unusual anatomy can show up with less obvious patterns. That is why stories about “I was told it was gastroenteritis, then my appendix ruptured” keep circulating. The takeaway is not to diagnose yourself from the couch. It is to respect pain that is worsening, localizing, or becoming impossible to ignore.
4. Pneumonia: The Flu’s Meaner Cousin
Pneumonia can feel like the flu, especially in the early stages. Fever, chills, fatigue, cough, nausea, and body aches can all overlap. What often separates pneumonia is the chest component: shortness of breath, chest pain when breathing or coughing, confusion in some adults, and a cough that becomes more intense or productive. Sometimes influenza itself leads to pneumonia, which makes things even trickier. The original diagnosis may not have been wrong so much as incomplete. A straightforward flu can become something more serious.
This is one reason the phrase “I was getting better, then suddenly worse” shows up so often in cautionary tales. Improvement followed by a setback is not always harmless. Sometimes it is the illness changing shape.
5. Pulmonary Embolism: The Silent Ambush
A pulmonary embolism, or blood clot in the lungs, can masquerade as flu, anxiety, or a bad chest infection. A person may notice shortness of breath, chest pain, lightheadedness, fatigue, sweating, or a rapid heartbeat. None of those symptoms comes with a flashing sign that says, “Hello, this is a clot.” That is what makes it dangerous.
In real-world misdiagnosis stories, pulmonary embolism often appears in the chapter titled “I knew something felt off.” The person may not look dramatically sick at first. They may just seem winded, shaky, or vaguely ill. But unexplained chest pain, sudden breathlessness, fainting, or a sharp drop in exercise tolerance is not a “wait a week and see” personality trait.
6. Heart Attack: Not Always the Hollywood Version
Heart attacks can present with chest pain, but not always in the classic way people expect. Some people, especially women, report unusual fatigue, nausea, sweating, upper back pain, jaw pain, shortness of breath, indigestion-like discomfort, or pressure in the chest or upper abdomen. That symptom cluster can look suspiciously like flu, reflux, or anxiety.
That is part of why so many memorable stories begin with, “I thought I had a virus” or “I assumed it was just stress.” The body does not always send elegant, cinematic messages. Sometimes it sends a vague memo in smudged ink.
7. Stroke: The One That Does Not Wait for Convenience
Stroke is not usually mistaken for the flu in the same way as pneumonia or sepsis, but atypical early symptoms can still confuse the picture. Dizziness, sudden weakness, trouble speaking, trouble walking, vision changes, confusion, or a severe headache may initially be downplayed as exhaustion, dehydration, migraine, or “just being sick.”
Stroke does not care whether the timing is inconvenient, whether it is a holiday weekend, or whether someone is trying very hard not to be dramatic. Sudden neurologic symptoms need urgent attention. The body is allowed to be subtle right up until it absolutely is not.
Why Misdiagnosis Stories Spread So Fast Online
Because they do two things at once. First, they validate a deeply unsettling truth: symptoms do not always behave. Second, they reflect a common patient fear of being dismissed. Many people are less afraid of getting sick than they are of not being believed while they are getting sick.
Research on diagnostic error has shown that missed, delayed, or incorrect diagnoses are a real patient-safety problem, especially when dangerous diseases present in nonclassic ways. Patient narratives often describe the same themes: symptoms that changed over time, communication that broke down, assumptions that stuck too long, and follow-up that happened too late. In plain English, people often feel that the first explanation got too comfortable and nobody kicked the tires hard enough after that.
To be fair, diagnosis is not fortune-telling. Medicine works with probability, patterns, tests, and timing. A person with fever and body aches in flu season may honestly look like they have the flu. But the best diagnosis is not a stubborn one. It is a flexible one.
Red Flags That Deserve Faster Medical Attention
If symptoms are changing, intensifying, or pairing up in alarming ways, it is time to stop negotiating with your sofa. Warning signs that deserve urgent evaluation can include:
- difficulty breathing or shortness of breath
- chest pain, chest pressure, or new upper back or jaw discomfort
- confusion, trouble waking up, or new mental status changes
- a stiff neck with fever or a severe headache
- one-sided weakness, speech trouble, fainting, or loss of balance
- abdominal pain that worsens, localizes, or becomes severe
- symptoms that briefly improve and then come roaring back worse than before
- extreme weakness, blue lips, dehydration, or an inability to keep fluids down
That does not mean every red flag guarantees catastrophe. It means the body has moved out of the “maybe a basic virus” lane and into “please get real eyes on this” territory.
How To Advocate for Yourself Without Turning Into Your Own Doom Blogger
Describe the timeline clearly
Doctors need the sequence. What started first? What got worse? What changed today? “I’ve had fever and cough for three days, but today I got chest pain and I’m short of breath walking across the room” is more useful than “I feel awful,” though both are true.
Name the weird part
Patients often bury the most alarming symptom under a pile of context. Lead with the odd detail: “I feel confused,” “I cannot catch my breath,” “the pain is now only on the lower right side,” or “I fainted.” That is not being dramatic. That is being efficient.
Ask what would make the diagnosis change
A good question is: What symptoms should make me come back immediately? Another good one is: If this is not improving, what else could it be? Those questions invite a safety net, which is a beautiful thing to have when bodies start improvising.
Respect your own baseline
If you are saying, “This feels different from any flu I’ve had before,” that matters. It is not proof of a diagnosis, but it is valuable information. People live in their bodies full-time. They notice when the script is off.
The Big Lesson Behind the Wildest Misdiagnosis Stories
The most important lesson is not that medicine is careless or that every viral illness hides a disaster. It is that serious conditions often begin with ordinary symptoms, and ordinary symptoms become dangerous when they are severe, fast-changing, or attached to the wrong companions.
In other words, the body loves reruns. Fever, fatigue, nausea, chills, cough, and body aches are not exclusive to one illness. What separates a routine flu from something far more dangerous is context, progression, and pattern. A diagnosis is not just a label slapped on a symptom list. It is a moving interpretation of a moving target.
So yes, people are sharing their wildest misdiagnosis stories. Some are dramatic. Some are heartbreaking. Some are told with gallows humor because laughter is cheaper than therapy. But behind all of them sits the same practical truth: when symptoms escalate, do not get sentimental about the original explanation. “Probably viral” is not a sacred oath. It is a starting point.
Experiences People Keep Sharing About “Flu Or Fatal” Mix-Ups
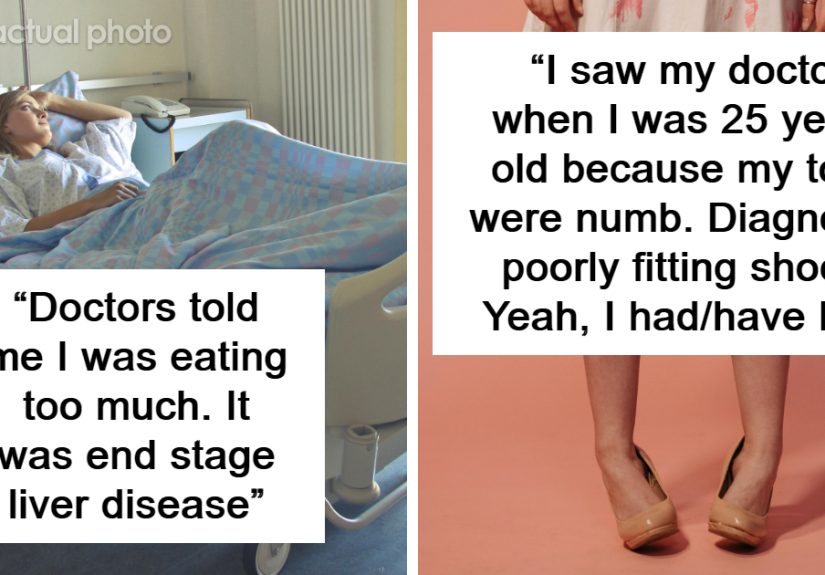
Across patient forums, health features, awareness campaigns, and first-person retellings, the stories follow remarkably similar patterns. One person says they went to urgent care with fever, aches, and a pounding headache and were told it was likely viral. They went home, took the recommended meds, tried to sleep, and woke up feeling not better but strangely worse: light hurt, their neck felt rigid, and even simple conversation took effort. In the retelling, the terrifying part is not just the diagnosis that came later. It is the memory of how normal the whole thing sounded at first.
Another common story starts in the stomach. Someone develops nausea, low fever, and a vague ache near the belly button. They assume stomach flu. A clinician may assume stomach flu too, especially if vomiting shows up early. But then the pain creeps lower, sharper, and more focused. The storyteller remembers the moment they realized this was no ordinary digestive tantrum. Usually it is described with some variation of, “I knew I was not being brave, I was being stupid.” That line appears so often because many people are taught to minimize pain until the pain becomes impossible to minimize.
Then there are the stories involving breathing. A person says they thought they had the flu because they felt wiped out, sweaty, and tight in the chest. Maybe there was a cough. Maybe there was not. Maybe they blamed stress, bad sleep, weather, or being out of shape. Later they learn it was pneumonia, a clot, or another serious cardiopulmonary problem. These stories are chilling because fatigue is such an easy symptom to wave away. America practically runs on people saying, “I’m tired, but it’s fine.” Sometimes it is not fine. Sometimes it is your body filing an urgent complaint in all caps.
Women’s stories about heart attacks often carry a special kind of disbelief. The symptoms may have sounded like indigestion, nausea, back pain, or crushing exhaustion rather than the classic chest-clutching stereotype. In many retellings, the most haunting detail is how long they talked themselves out of seeking care because the symptoms did not match the movie version of a heart emergency. The body, once again, had chosen ambiguity over drama.
What connects all these experiences is not that medicine always gets it wrong. It is that dangerous illnesses often arrive dressed as ordinary ones. People remember the mismatch between appearance and reality. They remember being told to monitor things and then discovering that “monitor” turned into “move now.” They remember how quickly a reasonable first guess became the wrong final answer.
That is why these stories keep spreading. They are not just tales of bad luck. They are reminders that worsening symptoms deserve re-evaluation, that red flags matter, and that getting help twice is better than needing help once too late. A flu-like illness can absolutely be just the flu. But when the pattern changes, the safest move is to change your thinking too.