Table of Contents >> Show >> Hide
- Why doctor visits feel shorter than ever
- What rushed appointments cost patients
- What rushed appointments cost doctors
- Why the problem feels even worse to patients
- How patients can get more out of a too-short visit
- What would actually make visits feel human again
- Real-life experiences: when “the doctor will see you now” feels like a race against the clock
- Conclusion
- SEO Tags
If modern health care had a slogan, it might be: Please hold, fill out these forms, update your portal password, and then try to explain your entire body in 14 minutes or less. That sounds like a joke, but for many Americans, it is uncomfortably close to the real experience of getting care. The appointment itself often feels brief, the waiting feels eternal, and the bill somehow still arrives with the confidence of a Broadway finale.
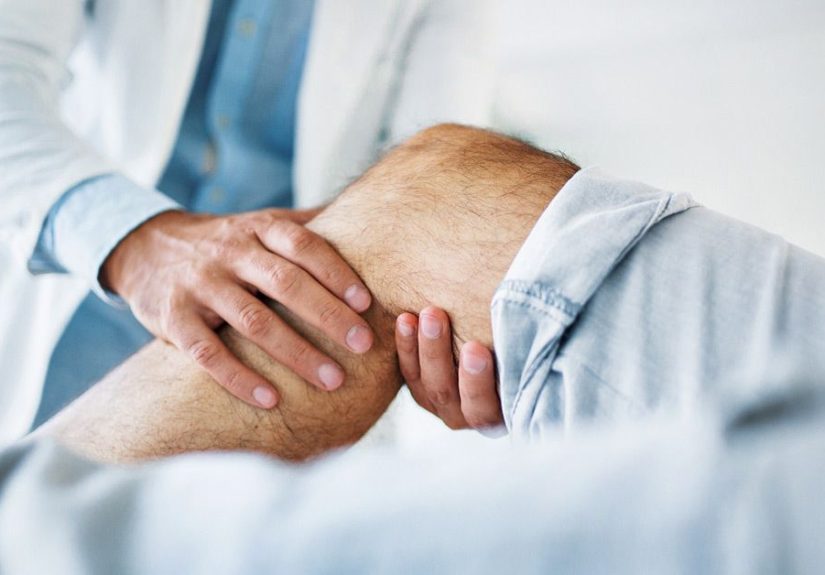
To be fair, most doctor visits are not literally one minute long. But the title captures something patients know in their bones: the visit can feel rushed, fragmented, and oddly transactional. You finally get in the room, sit on the paper-covered table that crinkles like a snack bag, and begin to explain why you are there. Then the clock starts sprinting. Before you reach concern number three, the visit is already drifting toward the exit.
This is not simply a bedside-manner issue. It is a systems issue. Short doctor visits are tied to the economics of American medicine, the growing complexity of patient care, the shortage of clinicians, the heavy burden of electronic records, and the pressure to move more people through the day. In other words, the problem is not that doctors do not care. It is that the structure around them often makes caring look suspiciously like speed dating with a stethoscope.
Here is why the modern medical visit can feel so short, what that costs patients and clinicians, and what would actually make the exam room feel human again.
Why doctor visits feel shorter than ever
There is simply more to do in the same amount of time
Primary care has become a juggling act with flaming torches. Today’s visit is rarely about one tidy issue. A single appointment may include blood pressure management, medication refills, preventive screenings, lab follow-up, insurance paperwork, mental health concerns, and one completely unrelated problem the patient almost forgot to mention until the hand is already on the doorknob.
That would be challenging enough if Americans were broadly healthy. We are not. Chronic disease is common, and often stacked. Many adults are managing multiple conditions at once, which means each visit carries more medical history, more medications, more questions, and more risk. The result is simple math: more complexity packed into the same fixed appointment slot.
Researchers have made this mismatch painfully clear. Estimates suggest primary care clinicians would need far more hours than exist in a normal workday to provide all recommended preventive, chronic, and acute care for a typical patient panel. That does not mean doctors are lazy. It means the demand placed on them is unrealistic. When the to-do list requires more time than the planet is offering, something gets compressed. Usually, that “something” is conversation.
The visit does not end when the patient leaves the room
One of the strangest truths about modern medicine is that the doctor-patient visit is only part of the doctor’s work. A huge share of the job happens inside the electronic health record. Documentation, order entry, messaging, refill requests, prior authorization headaches, inbox alerts, coding requirements, referrals, and compliance tasks all compete for time.
So while patients experience a short face-to-face encounter, clinicians often experience a long digital afterparty. Notes must be finished. Messages must be answered. Alerts must be cleared. Test results must be signed. Insurance paperwork must be appeased like a fussy Roman god. That administrative load can spill into lunch, evenings, and weekends.
This helps explain a paradox patients often feel but cannot name: “Why was my visit so short if my doctor seems so busy?” Because the visit is only one slice of the work. The exam room is the visible tip of an iceberg made of clicks.
Primary care is asked to do everything on a bargain budget
In the United States, primary care is enormously important and chronically under-supported. It is expected to prevent disease, manage chronic illness, coordinate specialists, monitor medications, handle referrals, answer portal messages, and keep people out of expensive emergency care. Yet it has historically received a relatively small share of total health spending compared with specialist and procedure-based care.
That imbalance matters. When a system pays more generously for procedures than for time, it quietly teaches organizations what to value. A careful conversation about symptoms, goals, risks, and follow-up may be the most useful part of a visit, but it is often not the part the payment structure rewards most strongly. The consequence is predictable: shorter visits, more volume, less breathing room.
There are not enough clinicians to meet demand
Even the best-designed schedule falls apart when there are too few people to do the work. The United States faces a continuing physician shortage, and primary care has been under particular strain. At the same time, the population is aging, chronic disease is common, and patient needs are becoming more complex rather than less.
That shortage shows up in the everyday experience of care. Patients wait longer for appointments. Practices close panels. Rural communities struggle to recruit clinicians. Urban systems cope with backlogs. And when access is tight, each available clinician is expected to carry more. Short visits do not happen in a vacuum. They happen in crowded systems.
What rushed appointments cost patients
A short visit is not automatically a bad visit. Some concerns are straightforward. A medication refill, a quick follow-up on a simple issue, or a minor acute problem may not require an epic bedside monologue. But when rushed care becomes the norm, the risks go up.
First, patients may leave with unanswered questions. That sounds mild, but it is not. Unanswered questions lead to confusion about medications, uncertainty about warning signs, missed follow-up, and lower confidence in the care plan. A patient may nod along in the room and then sit in the parking lot wondering what on earth just happened.
Second, shorter visits can make it harder to catch nuance. The story behind symptoms matters. A cough can be a cough, or it can be a clue. Chest discomfort can be heartburn, anxiety, or something much more serious. Good medicine often depends on detail, pattern recognition, and context. Those things do not always flourish in a rushed environment.
Third, time pressure can affect decisions. When there is little time to explain why an antibiotic is unnecessary, or why a sedating medication may be risky, a quick prescription can start to look dangerously convenient. That is one reason researchers continue to examine whether shorter visits are associated with lower-value or inappropriate prescribing in some settings.
Fourth, rushed care can weaken trust. Patients want more than a technically correct diagnosis. They want to feel heard. In fact, the patient-experience measures used in U.S. health care explicitly ask whether a clinician explained things clearly, listened carefully, showed respect, and spent enough time. That last one is telling. Even our official quality frameworks understand that time is not just a luxury. It is part of care.
What rushed appointments cost doctors
Patients are not the only ones frustrated by the speed of modern medicine. Doctors often dislike it too. Many entered medicine to solve problems, build relationships, and think carefully. Few dreamed of a career in box-checking while toggling between note templates and prior authorization forms.
Burnout remains a major issue in medicine, even if some recent measures have improved from the worst pandemic-era highs. And burnout is not just about long hours. It is about moral friction: the exhausting gap between the care clinicians want to give and the care the system realistically allows them to deliver.
That gap can be brutal. A doctor may know a patient needs a fuller conversation about weight loss, depression, caregiving stress, grief, sleep, or finances. But if the schedule is jammed, the inbox is exploding, and the chart still needs documentation, the visit can shrink into triage. Everyone leaves feeling slightly shortchanged. The patient thinks, “That was fast.” The doctor thinks, “I know.”
Why the problem feels even worse to patients
One reason patients feel especially irritated is that the short visit is only part of a much longer effort. Getting care can consume hours once travel, waiting, parking, forms, phone calls, and scheduling are counted. So even when face-to-face time averages around 18 to 20 minutes in many analyses, the total burden of obtaining care can be far higher.
That mismatch is emotionally potent. Nobody loves taking time off work, arranging transportation, sitting in a waiting room, and then getting five and a half minutes of eye contact before being told to “monitor symptoms.” The experience can feel like buying front-row concert tickets and then being seated behind a support pillar.
It also hits some patients harder than others. People with lower incomes, more complex medical needs, language barriers, difficult transportation, caregiving responsibilities, or unstable work schedules often face the greatest burdens. In that sense, rushed care is not just annoying. It can deepen inequality.
How patients can get more out of a too-short visit
Patients should not have to become project managers to receive basic medical care, but in the current system, a little strategy helps. The most effective move is usually to prioritize. Bring the top two or three concerns, not a verbal junk drawer. If something is urgent, say that early. If you need a medication decision, test interpretation, or a referral, say that clearly. Doctors cannot address what they do not know is most important.
It also helps to bring specifics. “I feel weird” is honest, but “I have had chest tightness for two weeks, it happens when I climb stairs, and it improves after I rest” is much more useful. Dates, symptom patterns, medication lists, home blood pressure readings, blood sugar logs, and photos of rashes can save valuable minutes.
Patients should also feel allowed to say, “I still have questions,” or “Can you explain what the next step is?” That is not rude. It is responsible. If a concern is too complex for one visit, asking for a dedicated follow-up is often smarter than trying to cram an entire season of medical drama into one episode.
What would actually make visits feel human again
Pay for time and continuity, not just throughput
If health systems want better primary care, they have to finance it like it matters. That means rewarding continuity, care coordination, prevention, chronic disease management, and relationship-based care rather than acting as though the only valuable medical event is a billable procedure with impressive equipment.
Use team-based care for real, not as a buzzword
Team-based care is not medical jargon for “good luck, everybody.” Done well, it means nurses, pharmacists, behavioral health clinicians, dietitians, medical assistants, care coordinators, and documentation support all help deliver care at the top of their training. That can free physicians to focus on the parts of the visit that truly require physician judgment. It can also give patients a more complete experience instead of a hurried one-person show.
Reduce documentation burden instead of worshipping it
Not every click is sacred. Some documentation is essential. A lot of it is defensive, redundant, or designed to satisfy billing logic rather than patient need. Health systems that reduce unnecessary clerical work, improve EHR design, or meaningfully support documentation can give clinicians something radical: time.
Expand access outside the classic office visit
Better follow-up through messaging, telehealth, remote monitoring, after-hours access, and home-based care can take pressure off the traditional in-office appointment. The goal is not to replace human visits with apps. It is to reserve in-person time for the moments when in-person care matters most.
Real-life experiences: when “the doctor will see you now” feels like a race against the clock
Imagine a working parent who finally gets an appointment after weeks of trying. She has taken time off, arranged child care, and driven across town. In the waiting room, she fills out forms she swears she already completed online. When the doctor arrives, she wants to discuss fatigue, a medication side effect, rising blood pressure, and the fact that she has not slept well in months. Instead, the visit narrows almost immediately to the blood pressure reading. It is not that the other concerns are unimportant. It is that there is only so much room in the visit, and something has to be pushed to “next time.” She leaves with a new prescription, but not with the sense that the full story was heard.
Now picture an older adult with diabetes, arthritis, and heart disease. He arrives with a careful list because he knows from experience that memory gets slippery in the exam room. He wants to ask about foot numbness, test results, dizziness, and whether one medication is making him feel foggy. The physician is kind, but visibly rushed. There are labs to review, medications to reconcile, screenings to discuss, and a referral to place. By the end, the major medical boxes are checked, but the dizziness discussion never quite gets the oxygen it deserves. Nothing catastrophic happened. Yet the patient still senses that the visit was more efficient than reassuring.
Clinicians feel the same pressure from the other side. A family physician may have a schedule packed every 15 or 20 minutes, plus an inbox full of refill requests, portal messages, school forms, FMLA paperwork, and prior authorizations waiting between visits. In one room is a teenager with anxiety. In another is a retiree with worsening shortness of breath. In another is a patient who mainly needs someone to sit down and explain what the specialist said last week. The doctor may want to linger, clarify, reassure, and educate. But if each visit runs long, the entire day collapses, and every patient after lunch feels the domino effect.
This is why so many patients say, “My doctor barely spent any time with me,” while so many doctors say, “I am working nonstop.” Both things can be true. The patient experiences a compressed conversation. The doctor experiences an overflowing workload that extends beyond the visible appointment. The mismatch creates resentment on both sides even though neither side is really the enemy.
And then there is the emotional residue. Patients may hesitate to bring up embarrassing symptoms because the room feels rushed. They may avoid asking for clarification because they do not want to seem difficult. Doctors may feel they delivered medically competent care while still falling short of humane care. Over time, these tiny disappointments add up. One hurried visit might be manageable. A health system built on hurried visits starts to feel lonely.
Conclusion
The real scandal is not that some appointments are short. It is that a country capable of astonishing medical innovation still so often makes basic primary care feel hurried, fragmented, and hard to access. Americans spend a great deal on health care, yet many still wait too long, pay too much, and receive too little face-to-face time when they finally get in the room.
So yes, the doctor will see you now. But the bigger question is whether the system will let that visit feel like care instead of compressed logistics. If we want appointments that feel less rushed, the answer is not simply “tell doctors to slow down.” The answer is to redesign the environment around them: invest in primary care, reduce administrative drag, expand team-based support, pay for continuity, and treat time as a clinical resource rather than a luxury add-on.
Because in medicine, a few more minutes can mean a better explanation, a safer decision, an earlier diagnosis, a stronger relationship, and a patient who leaves feeling less like a number and more like a person. That is not a small upgrade. That is the point.